INTRODUCTION
Intussusception is the most common cause of pediatric small bowel obstruction. It occurs predominantly in 3 to 36 month old males1 and the annual incidence is approximately 56 cases per 100,000 cases.2 In contrast to adult intussusception, 2%-12% of intussusception cases in children contain a lead point such as Meckel’s diverticulum.3 “Currant jelly stools” are commonly misconceived to be a frequent finding. However, this late marker of bowel ischemia is found in only a minority of cases.3,4 Since history is limited in nonverbal children, the burden of diagnosis relies on a careful physical exam and particular attention to overall appearance, lethargy or inconsolability of the infant. Even then, the classic presentation is not reliable, particularly in cases of small bowel obstruction.3 computerized tomography (CT) and ultrasound (US) is diagnostic; however, ultrasound has the advantage of limiting radiation exposure. Availability of bedside point of care ultrasound (POCUS) to diagnose uncharacteristic cases of intussusception could prevent delay of diagnosis. Classically in the United States, ultrasound is performed by an ultrasound technician or radiologist.5 It has not yet been widely adopted that a bedside point of care ultrasound (POCUS) by an emergency provider can replace a formal ultrasound by radiology if determined negative. However, studies indicate specificity of POCUS by emergency providers is approaching 100%.5 Identification of an intussusception on POCUS could greatly impact the speed of disposition, particularly in departments without ultrasound and radiology available overnight. The diagnosis is made noting a “bulls eye” or “target” appearance6 in transverse view, created by invagination of the intussusceptum (proximal bowel) into the intussuscepiens (distal segment).2 Early surgical intervention versus enema treatment is essential to limit morbidity and mortality.
CASE REPORT
A 13-month-old African-American male with a chief complaint of persistent vomiting for one day presented to the emergency department with his mother. The patient’s mother reported 9 episodes of vomiting that was associated with irritability and the patient’s pulling of his knees up to his chest. Vomiting was exacerbated with any feedings. His last fluid intake and wet diaper were the morning of presentation and both were decreased from baseline. The vomits was non-bloody, non-bilious, and not projectile. His last bowel movement was diarrhea without blood or melena and occurred the day before. There were no known sick contacts, recent travel, illness, fever, rash, prior conditions, medications, birth complications, or surgeries.The patient was fully immunized. No home therapies were attempted. Vital signs include a heart rate of 111, respiratory rate 20, blood pressure 94/51, mean arterial pressure 65, and his weight was 11.8 kg. On physical examination the patient was noted to be alert, nontoxic and in no acute distress. The abdomen was soft with slight fullness to palpation of the right upper quadrant (RUQ) but no appreciable mass was palpated. The bowel sounds were normal and no organomegaly was noted. On palpation of the abdomen the infant cried, but otherwise the examination was normal. On rectal examination no bloody or melanotic stool was noted in the rectal vault, but the fecal occult test was positive. A radiograph of the abdomen revealed a paucity of cecal air. (Figure 1) Bedside ultrasound images were obtained. (Figure 2)
Figure 1: Paucity of Air on Acute Abdominal Series.
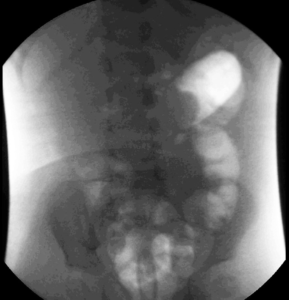
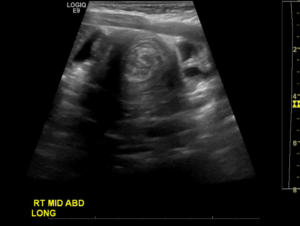
Figure 2: Abdominal Ultrasound Demonstrating the Target or Bulls Eye Sign Characteristic of Intussusception.
DISCUSSION AND CONCLUSIONS
Even though the details of CT scan are superior,3 ultrasound should be attempted initially for diagnosis. Sensitivity and specificity of ultrasound for intussusception approaches 100% with an experienced sonographer.3,7 Accuracy of diagnosing an intussusception in the ED by a novice provider can be improved with didactic and focused training following the techniques for success outlined in Table 1.5 Early intervention is key and is expedited by ultrasonographic diagnosis. The longer the bowel intussusception persists beyond 24 hours, the less chance that an air or contrast enema will successfully reduce it.2 Surgical intervention should be considered early if the patient is unstable with suspected perforation or if enema treatment fails.2
| Table 1: Techniques for Successful Ultrasound. |
| Techniques for Successful Ultrasound |
| 1. Use a linear transducer (5-10 MHz) |
| 2. Apply sufficient amount of ultrasound gel to easily sweep between locations |
| 3. Start in the right lower quadrant, transverse orientation with the indicator pointed to the patient’s right |
| 4. Identify the psoas as your starting landmark |
| 5. Adjust the depth appropriately |
| 6. Sweep superiolaterally toward the gallbladder and liver landmarks |
| 7. In the right upper quadrant, rotate 90 degrees clockwise (indicator toward patient’s head) |
| 8. Sweep across the epigastrium to the left upper quadrant in longitudinal orientation |
| 9. Rotate the transducer counter clockwise 90 degrees in the left upper quadrant and sweep inferiorly to the left lower quadrant. |
CONFLICTS OF INTEREST
The authors have no conflicts of interest, sources of funding or support, disclaimers, credits, other information and acknowledgement to disclose.
FUNDING
No funding source was necessary in the creation of this case report.