1. Royal College of Radiologists (Great Britain). iRefer: Making the best Use of Clinical Radiology. London, UK. The Royal College of Radiologists; 2016: 207.
2. Kellow ZS, Macinnes M, Kurzencwyg D, et al. The role of abdominal radiography in the evaluation of the nontrauma emergency patient. Radiology. 2008; 248(3): 887-893. doi: 10.1148/radiol.2483071772
3. Anyanwu AC, Moalypour SM. Are abdominal radiographs still overutilized in the assessment of acute abdominal pain? A district general hospital audit. J R Coll Surg Edinb. 1998; 43(4): 267-270.
4. Field S, Guy PJ, Upsdell SM, Scourfield AE. The erect abdominal radiograph in the acute abdomen: should its routine use be abandoned? Br Med J (Clin Res Ed). 1985; 290(6486): 1934-1936. doi: 10.1136/bmj.290.6486.1934
5. Morris-Stiff G, Stiff RE, Morris-Stiff H. Abdominal radiograph requesting in the setting of acute abdominal pain: temporal trends and appropriateness of requesting. Ann R Coll Surg Engl. 2006; 88(3): 270-274. doi: 10.1308/003588406X98586
6. Mackersie AB, Lane MJ, Gerhardt RT, et al. Nontraumatic acute abdominal pain: Unenhanced helical CT compared with three-view acute abdominal series. Radiology. 2005; 237: 114-122. doi: 10.1148/radiol.2371040066
7. Gupta K, Bhandari R, Chander R. Comparative study of plain abdomen and ultrasound in non-traumatic acute abdomen. Indian J Radiol Imaging. 2005; 15(1): 109-115. doi: 10.4103/0971-3026.28760
8. Ahn SH, Mayo-smith WW, Murphy BL, Reinert SE, Cronan JJ. Radiology abdominal pain in adult patients: Abdominal radiography compared with CT evaluation 1. Radiology. 2002; 225: 159-164.
9. Tsalafoutas IA, Koukourakis GV. Patient dose considerations in computed tomography examinations. World J Radiol. 2010; 2(7): 262-268. doi: 10.4329/wjr.v2.i7.262
10. Beckmann EC. CT scanning the early days. Br J Radiol. 2006; 79(937): 5-8. doi: 10.1259/bjr/29444122
11. Christner J, Kofler J, McCollough C. Estimating effective dose for CT using dose–length product compared with using Organ doses: Consequences of adopting international commission on radiological protection publication 103 or Dual-Energy Scanning. Med Phys Informatics. 2010; 194: 881-889. doi: 10.2214/AJR.09.3462
12. Yeh D, Tsai H, Tyan Y, Chang Y. The population effective dose of medical computed tomography examinations in Taiwan for 2013. PLoS One. 2016; 11(10): e0165526. doi: 10.1371/journal.pone.0165526
13. Huda W, Ogden KM, Khorasani MR. Converting dose-length product to effective dose at CT. Radiology. 2008; 248(3): 995-1003. doi: 10.1148/radiol.2483071964
14. Ware DE, Huda W, Mergo PJ, Litwiller AL. Radiation effective doses to patients undergoing abdominal CT examinations 1. Med Phys. 1999; 210(8): 645-650. doi: 10.1148/radiology.210.3.r99mr05645
15. Tamm EP, Rong XJ, Cody DD, Ernst RD, Fitzgerald NE, Kundra V. Quality initiatives: CT radiation dose reduction: How to implement change without sacrificing diagnostic quality. Radio Graphics. 2011; 31(7): 1823-1832. doi: 10.1148/rg.317115027
16. Lin EC. Radiation risk from medical imaging. Mayo Clin Proc. 2010; 85(12): 1142-1146; quiz 1146. doi: 10.4065/mcp.2010.0260
17. Gans SL, Stoker J, Boermeester MA. Plain abdominal radiography in acute abdominal pain; past, present, and future. Int J Gen Med. 2012; 5: 525-533. doi: 10.2147/IJGM.S17410
18. Osei EK, Darko J. A survey of organ equivalent and effective doses from diagnostic radiology procedures. ISRN Radiol. 2013; 2013. doi: 10.5402/2013/204346
19. Van Unnik JG, Broerse JJ, Geleijns J, Jansen JT, Zoetelief J, Zweers D. Survey of CT techniques and absorbed dose in various Dutch hospitals. Br J Radiol. 1997; 70(832): 367-371. doi: 10.1259/bjr.70.832.9166072
20. Smith-Bindman R, Lipson J, Marcus R, et al. Radiation dose associated with common computed tomography examinations and the associated lifetime attributable risk of cancer. Arch Intern Med. 2009; 169(22): 2078-2086. doi: 10.1001/archinternmed.2009.427
21. Karkhanis S, Medcalf J. Plain abdomen radiographs: The right view? Eur J Emerg Med. 2009; 16(5): 267-270. doi: 10.1097/MEJ.0b013e328323d6e5
22. Smith JE, Hall EJ. The use of plain abdominal x rays in the emergency department. Emerg Med J. 2009; 26(3): 160-163. doi: 10.1136/emj.2008.059113
23. Miller G, Boman J, Shrier I, Gordon PH. Etiology of small bowel obstruction. Am J Surg. 2000; 180(1): 33-36. doi: 10.1016/S0002-9610(00)00407-4
24. Maglinte DD, Balthazar EJ, Kelvin FM, Megibow AJ. The role of radiology in the diagnosis of small-bowel obstruction. AJR Am J Roentgenol. 1997; 168(5): 1171-1180. doi: 10.1016/S0002-9610(00)00407-4
25. Shrake PD, Rex DK, Lappas JC, Maglinte DD. Radiographic evaluation of suspected small bowel obstruction. Am J Gastroenterol. 1991; 86(2): 175-178.
26. Maglinte DD, Reyes BL, Harmon BH, et al. Reliability and role of plain film radiography and CT in the diagnosis of small-bowel obstruction. AJR Am J Roentgenol. 1996; 167(6): 1451-1455. doi: 10.2214/ajr.167.6.8956576
27. Frager D, Medwid SW, Baer JW, Mollinelli B, Friedman M. CT of small-bowel obstruction: value in establishing the diagnosis and determining the degree and cause. AJR Am J Roentgenol. 1994; 162(1): 37-41. doi: 10.2214/ajr.162.1.8273686
28. Suri S, Gupta S, Sudhakar PJ, Venkataramu NK, Sood B, Wig JD. Comparative evaluation of plain films, ultrasound and CT in the diagnosis of intestinal obstruction. Acta Radiol. 1999; 40(4): 422-428. doi: 10.3109/02841859909177758
29. Gazelle GS, Goldberg MA, Wittenberg J, Halpern EF, Pinkney L, Mueller PR. Efficacy of CT in distinguishing small-bowel obstruction from other causes of small-bowel dilatation. AJR Am J Roentgenol. 1994; 162(1): 43-47. doi: 10.2214/ajr.162.1.8273687
30. Mullan CP, Siewert B, Eisenberg RL. Small Bowel Obstruction. AJR Am J Roentgenol. 2012; 198(2): W105-W117. doi: 10.2214/AJR.10.4998
31. Stoker J, van Randen A, Laméris W, Boermeester MA. Imaging patients with acute abdominal pain. Radiology. 2009; 253(1): 31-46. doi: 10.1148/radiol.2531090302
32. Hayakawa K, Tanikake M, Yoshida S, Urata Y, Yamamoto E, Morimoto T. Radiological diagnosis of large-bowel obstruction: neoplastic etiology. Emerg Radiol. 2013; 20(1): 69-76. doi: 10.1007/s10140-012-1088-2
33. Jaffe T, Thompson WM. Large-bowel obstruction in the adult: classic radiographic and CT findings, etiology, and mimics. Radiology. 2015; 275(3): 651-663. doi: 10.1148/radiol.2015140916
34. Ogata M, Imai S, Hosotani R, Aoyama H, Hayashi M, Ishikawa T. Abdominal sonography for the diagnosis of large bowel obstruction. Surg Today. 1994; 24(9): 791-794. doi: 10.1007/bf01636308
35. Frager D, Rovno HD, Baer JW, Bashist B, Friedman M. Prospective evaluation of colonic obstruction with computed tomography. Abdom Imaging. 23(2): 141-146. doi: 10.1007/s002619900307
36. Beattie GC, Peters RT, Guy S, Mendelson RM. Computed tomography in the assessment of suspected large bowel obstruction. ANZ J Surg. 2007; 77(3): 160-165. doi: 10.1111/j.1445-2197.2006.03998.x
37. Guniganti P, Bradenham CH, Raptis C, Menias CO, Mellnick VM. CT of gastric emergencies. Radio Graphics. 2015; 35(7): 1909-1921. doi: 10.1148/rg.2015150062
38. Solis C V, Chang Y, De Moya MA, Velmahos GC, Fagenholz PJ. Free air on plain film: Do we need a computed tomography too? J Emerg Trauma Shock. 2014; 7(1): 3-8. doi: 10.4103/0974-2700.125631
39. Levine MS, Scheiner JD, Rubesin SE, Laufer I, Herlinger H. Diagnosis of pneumoperitoneum on supine abdominal radiographs. AJR Am J Roentgenol. 1991; 156(4): 731-735. doi: 10.2214/ajr.156.4.2003436
40. Chen SC, Yen ZS, Wang HP, Lin FY, Hsu CY, Chen WJ. Ultrasonography is superior to plain radiography in the diagnosis of pneumoperitoneum. Br J Surg. 2002; 89(3): 351-354. doi: 10.1046/j.0007-1323.2001.02013.x
41. Cho KC, Baker SR. Extraluminal air. Diagnosis and significance. Radiol Clin North Am. 1994; 32(5): 829-844.
42. Braccini G, Lamacchia M, Boraschi P, et al. Ultrasound versus plain film in the detection of pneumoperitoneum. Abdom Imaging. 1996; 21(5): 404-412. doi: 10.1007/s002619900092
43. Maniatis V, Chryssikopoulos H, Roussakis A, et al. Perforation of the alimentary tract: Evaluation with computed tomography. Abdom Imaging. 2000; 25(4): 373-379. doi: 10.1007/s002610000022
44. Sherck J, Shatney C, Sensaki K, Selivanov V. The accuracy of computed tomography in the diagnosis of blunt small-bowel perforation. Am J Surg. 1994; 168(6): 670-675. doi: 10.1016/S0002-9610(05)80142-4
45. Singh JP, Steward MJ, Booth TC, Mukhtar H, Murray D. Evolution of imaging for abdominal perforation. Ann R Coll Surg Engl. 2010; 92(3): 182-188. doi: 10.1308/003588410X12664192075251
46. Hainaux B, Agneessens E, Bertinotti R, et al. Accuracy of MDCT in predicting site of gastrointestinal tract perforation. AJR Am J Roentgenol. 2006; 187(5): 1179-1183. doi: 10.2214/AJR.05.1179
47. Imuta M, Awai K, Nakayama Y, et al. Multidetector CT findings suggesting a perforation site in the gastrointestinal tract: Analysis in surgically confirmed 155 patients. Radiat Med. 2007; 25(3): 113-118. doi: 10.1007/s11604-006-0112-4
48. National Health Service. NHS Imaging and Radiodiagnostic activity in England. 2013. Web site. http://www.england.nhs.uk/statistics/wp-content/uploads/sites/2/2013/04/KH12-release-2012-13.pdf. Accessed June 20. 2017
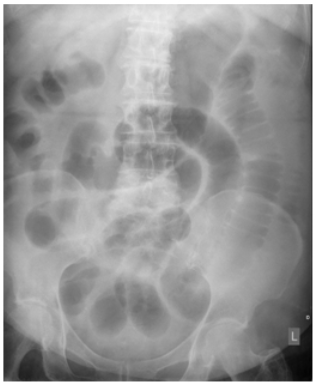
49. Bickle I. Small bowel obstruction. Radiopaedia.org; rID 33226. Web site. https://radiopaedia.org/cases/small-bowel-obstruction-12. Accessed June 20. 2017.
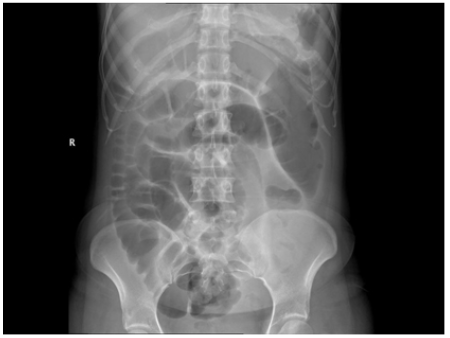
50. Babu V. Large bowel obstruction. Radiopaedia.org; rID 18015. Web site. https://radiopaedia.org/cases/large-bowel-obstruction. Accessed June 20. 2017.
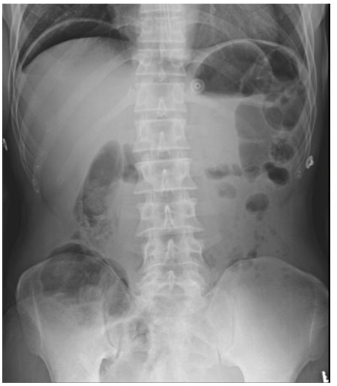
51. Kulkarni R. Bowel perforation. Radiopaedia.org; rID 21444. Web site. https://radiopaedia.org/cases/bowel-perforation. Accessed June 20. 2017.