INTRODUCTION
Horns are the pairs of hard, bonelike, permanent growth projecting from the head of cattle. They grow from a unique area of skin cells at the base of the horn. At about two months of age, horns become attached to the frontal bone of the skull.1A sinus lies within the skull beneath the horn bud. As the horn grows and attaches to the skull, this frontal sinus joins into the adjacent portion of the horn.2Dehorning or disbudding is the process of removing or stopping the growth of the horns and horn producing tissues after the horns have formed from the bud by different methods which can match to the size of the horn and the age of the animal for optimum effectiveness.3 The principal reason for dehorning is to remove the risk of injury to other animals in the herd or to people working with the cattle. If the calves are dehorned at an early age, the nutrients will be utilized for growth of the animal. Introducing a horned animal in a polled herd is poor judgment and cows with horns often sell at reduced prices.4
The horns of cattle are the unique adaptations of the skin. The horn generating cells are located between the junction of horns and skin known as the corium, which is the site for horn growth.5 Normally, horns begin as buds within the skin of the poll. At approximately 2-months of age, the horn buds become attached to the periosteum of the frontal bone overlying the frontal sinus. As the horns grow, the cornual diverticulum of the caudal portion of the frontal sinus extends into the most proximal portion of the horn.6 The cornual nerve, a branch of the trigeminal nerve (cranial nerve V), provides sensation to the skin of the horn/horn bud region. Injection of a local anesthetic around the cornual nerve as it traverses the frontal crest and desensitizes the area.7,8
If dehorning is not properly done with the removal of the whole corium, then horns can start regrowing.9 Similarly, improper dehorning especially, at an older age, predisposes to frontal sinusitis in the calves.10 Infection is a possible complication arising from dehorning, but this occurs mostly following invasive procedures that expose the sinus cavity to the external contaminated environment. Furthermore, the use of a surgical and a non-surgical instrument, including knives, Barnes dehorners, obstetrical wires, keystone (guillotine) dehorners, and saws may increase the risk of infection during dehorning.11
Normally, the wounds heal well with due care of postoperative treatment following dehorning. However, the procedure may cause several post-operative complications including bleeding, bacterial infections and fly contamination unless closely monitored. Operative animal requires 30-60-minutes for bleeding observation after dehorning but can be controlled through tourniquets, clamps or electric cauterizing. Not only these but also fly repellent should be provided for prevention of fly contamination, for 10-14-days.12 Besides that, sinusitis is a complication of dehorning and an exclusive risk in older calves.3 Sinusitis in cattle typically involves the frontal or maxillary sinus. Frontal sinusitis is generally associated with dehorning and maxillary sinusitis with infected teeth.13 This case report is aimed to describe the surgical management of horn in cow due to frontal sinusitis as a sequel to the trial of dehorning by sharp material is described.
CASE REPORT
Case History and Clinical Examination
Six-years-old healthy local breed cow with a medium body condition was presented to Hidi veterinary clinic one month before and referred to the Veterinary Teaching Hospital (VTH), Addis Ababa University, Ethiopia. In the former veterinary clinic, the cow was treated with oxytetracycline injection (20 mg/kg) intramuscularly for three days at one-day interval but after one month, pus was oozing out of the wound without regressing. After two weeks, the owner understood that the wound did not heal properly and the dehorned site was septic and finally referred to VTH. The owner also complained of discharging of pus around the right horn following trauma around the base of the horn by sharp instrument (knife) for dehorning purpose at their home. When clinically examined, the right horn was partially sawed (cut) but the majority of the horn structure is intact and there was oozing of unpleasant discharge (serous to purulent) through the opening as shown in (Figure 1A).
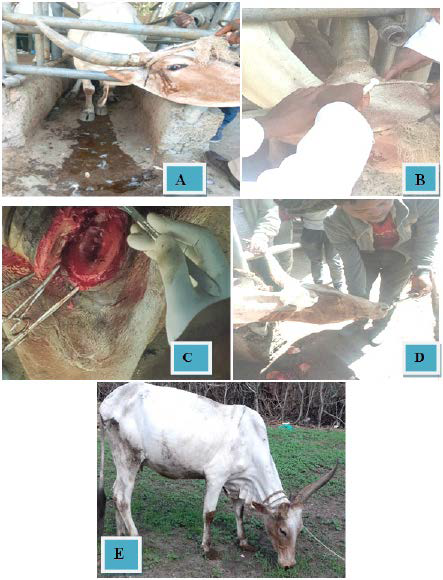
Figure 1. Dehorning and Its Surgical Procedure in Local Breed of Cow
A) Presentation of Case
B) Administration of Lidocaine to Block Cornual nerve C) Cutting the Injured Horn
D) Putting Bandage on Dehorned Horn Base E) After Four Months of Surgical Treatment
The cow tries to mutilate her horn by rubbing against inanimate object frequently. The depth of the affected horn would measure approximately (3 cm in diameter×6 cm in depth) and was observed near the base of the right horn. There was swelling and pain with signs of vocalization on palpation of the wound area. Further close examination of vital organ parameters such as heart rate, respiratory rate, pulse rate and mucous membrane revealed within physiological limits. Finally, based on the history and clinical observation, the case was diagnosed as suppurative frontal sinusitis and decided to be managed surgically by unilateral horn amputation.
Pre-operative Preparation of the Cow
The cow was restrained adequately and the circumferential skin surface of the base of the right horn was prepared aseptically by washing with soap and water. Then the hair was shaved with blade and cleansed thoroughly with diluted Chlorhexidine solution. Finally, the area was scrubbed with iodine solution and dried before readying for dehorning.
Anesthesia and Animal Control
The cow was properly immobilized with the combination of physical and chemical method. Physically, the cow was handled with bull Handle assisted by personnel and kept in the well-built crush which adequately restrains the cow. Chemically, the cow was regionally anaesthetized with two percent lidocaine (2% lidocaine hydrochloride, jeil pharm. co. Ltd., Korea), loaded in a syringe with 18 gauge, 1-1.5 inch needle, 6 ml/side is injected halfway between the lateral canthus of the orbit on upper third and base of the horn just under the shaft of frontal crest to block the cornual nerve (Figure 1B) and waited for 5-minutes. In addition, the cow was sedated with diazepam (manufactured by Intas pharmaceutical Ltd., India) @ 0.1 mg/kg I.M.
Surgical Correction and Treatment
After well securing, managing and keeping the cow on appropriate direction, elliptical skin incisions with a distance of approximately (~1 cm wide) around the base of the right horn was done for successful removal of corium (Figure 1C). Then active bleeding was occluded by tamponade and ligation of major vessels in addition to splashing with adrenaline on bleeding site. Further, the skin was bluntly and gently detached from the bone by scissor and retracted rostrally to get the skin flap and make it easy for sawing the horn. Thence after adequately exposing the proximal part of the bone and horn base, the base of the horn below the corium was cut with dehorning saw and the subcutaneous tissues hanging the detached horn were cut by surgical and removed with the corium.
After that, the frontal sinus was exposed and detected for any gross pathological findings (Figure 1C). Upon holding and lowering of the dehorned horn part to one side and an intact one to upper side there was a little cascade of clear to serous discharge from the cavity. Then the cavity was washed with sterilized water and cleaned with gauze. Skin edges were partially opposed to assist the skin contraction by using the silk 2-0 size in horizontal interrupted mattress. The area was properly bandaged with elastic bandages as a second layer after well padding the opening with cotton sandwiched in between large gauze and soaking with weak iodine solution as a primary layer. The area was properly secured to the normal horn and admitted home (Figure 1D).
Post-operative Care and Outcome
Sporadic bleeding was noticed following the horn amputation but it is normal and helps to clean the wound unless continued for a long period. As there was a difficulty to oppose the skin flap completely following horn amputation, it was properly bandaged with elastic bandages and dressed regularly. The dressing of the wound was done at three, fifth, seventh days up to fourteen days until healed. Penicillin (24 mg/kg) and dihydrostreptomycin sulphate (30 mg/kg) (Pen & Strep® Norbrook, UK) was also administered I.M. for four days post-operation at Hidi veterinary clinic. Fly repellant was also done around the wound by using sterile vaseline. The owner was also advised to avoid leaving the cow in the yard after dehorning but advised to supplement good nutrition to facilitate wound healing. After two months, the wound was healed completely and at four months of follow-up the cow improved in body weight (Figure 1E).
DISCUSSION AND CONCLUSION
Dehorning is a delicate procedure that requires professional skill and expertise because poor technique and management of wounds may result in ample complications that will lead to septicemia and may leads to death of the animal in addition to delayed healing.9Several dehorning methods such as using chemical agents, including sodium hydroxide and calcium hydroxide are commonly used for the purpose of burning the corium.4 Similarly, the electric hotiron device is also used on calves up to twelve weeks of age. However, this method has certain drawbacks as it is also considered to be relatively painful. But in adult ones, it is not advisable rather using other methods such as dehorning wire and saw after administering appropriate local anesthesia and sedation.13 This agrees with the current case management in terms of age and surgical management.
During dehorning, the removal of the skin corium by cutting with the detached horn is crucial unless it will re-grow again and promote infection in the unhealed wound.11 This also agrees with present case where dehorning was performed in which the corium was properly removed and healed after few months. Some research also reported that the use of Barnes dehorners, knives, Burners, tubes, guillotine dehorners, saws and obstetrical wire, all may increase the risk of infection after dehorning.10,14 In this case, the farmer used a knife to dehorn the cow and complications arose from the improper procedure, resulting in the development of frontal sinusitis.
Furthermore, the infected wound was not properly treated and managed except for the administration of systemic antibiotics. During dehorning, some behavioral signs observed include: head movement, tail wagging, tripping and rearing.11 However, head rubbing, head shaking, extension of the neck, ear and tail flicking and reduced rumination are postoperative signs. Which agrees with the earlier signs reported by Sutherland et al.15 In this case report, due to the infection of the wound, there was unpleasant discharges and pain with signs of reaction and reluctance to touch them as a result of the discomfort without prior administration of analgesic drugs. This disagrees with similar case management by systemic analgesic (Flunixine meglumine) administration to reduce the pain and inflammation as reported previously.13
The post-operative management of dehorning is very important in preventing bacterial contamination of the wound. Dehorning has been shown to increase the incidence of developing the Bovine papillomavirus, Bovine leucosis virus and Tetanus. Pre or post use of non-steroidal analgesics has proven effective in reducing pain and swelling in the dehorned site.12 In this case, no analgesic or suitable antibiotic medications were instituted by the owner, resulting in suppurative infection of the frontal sinus. However, proper wound management and medication was able to resolve the infection and ensured the healing process.
To sum up, surgical method of amputating horn is removal of the horn especially in adult animals at the base mainly below the corium when it is difficult to treat. But the procedure is highly invasive as the post-operative complications are high unless closely monitored and treated. In addition, the procedure is also highly complicated due to high probability of bleeding and delayed time of healing; predisposing the animal to infection of brain and myiasis. In this particular case report, the horn was surgically excised under aseptic condition and alleviation of pain through cornual nerve block. Finally, after removing the horn, the incision site was regularly dressed and bandaged and recovered after few months. So, for early recovery and positive outcome of the procedure, it should be managed early and regularly monitored for progression of healing.
ACKNOWLEDGEMENTS
The figures used in the case report belong to the author’s, captured in photograph while the author’s were conducting the surgical procedure. The Addis Ababa University college of Veterinary Medicine and Agriculture ethical review committee had critically reviewed the proposal in the context of research ethics and conclude that, there was no ethical problem. The case report was conducted at a certain Veterinary Teaching Hospital without any additional fund and prepared as surgical case report for learning and teaching of professionals across the world especially for veterinarians with your cooperation for processing and publication.
CONFLICTS OF INTEREST
The authors declare that they have no conflicts of interest.






