INTRODUCTION
The accumulation of advanced glycation end-products (AGEs) on tissue proteins has been implicated in the ageing of proteins and the progression of chronic age-related diseases such as atherosclerosis, chronic renal failure, Alzheimer’s disease and diabetes mellitus.1 AGEs and oxidative stress (OS) are two main contributors to the development of diabetic complications. AGEs represent a heterogeneous substance class, produced through nonenzymatic glycation of proteins, lipids or nucleic acids within the so-called Maillard reaction (MR).1,2
The formation and accumulation of AGEs on long-lived proteins affects the structure and function of proteins, enhances cytokine production and activates transcription factors via binding to specific receptors.2,3 In diabetes mellitus, AGEs accumulation in skin collagen is correlated both with the duration and severity of hyperglycaemia, and with the presence of long-term complications.2,3
In a diabetes control and complications trial (DCCT) sub-study, skin AGEs levels could account for 19-36% of the variance in incidence of long-term diabetic complications in intensively treated and for 14-51% in conventionally treated patients. The above indicate that tissue AGEs accumulation may reflect the cumulative effect of hyperglycemia and oxidative stress over many years.3,4,5 Simple quantitation of AGEs accumulation in tissue could provide a tool for assessing tissue injury and the risk of long-term complications.
Circulating or tissue-bound AGEs can be measured using enzyme-linked immunosorbent assay (ELISA), fluorescence spectroscopy, fluid chromatography and gas chromatography with mass spectrometry.5 Biochemical and immunochemical assays measure AGEs, like pentosidine, and carboxymethyl-lysine (CML). These methods are complex, invasive and highly costed. The measurement of tissue-bound AGEs is more stable, than the circulating AGEs. In particular, tissues with a slow turnover as the skin, display a high AGEs accumulation and are therefore most suitable for AGEs assessment.
The skin represents the most accessible tissue for AGEs measurements, with the biochemical analysis of skin biopsies constituting the golden standard. However, this method is invasive, expensive, requires analysis in specialized centres. A growing interest in the non-invasive assessment of AGEs existed lately and non-invasive, quick, reproducible and relatively low cost methods were developed. The skin autofluorescence method (SAF) is a non-invasive quick and reliable method, based on the autofluorescent properties of some (e.g., pentosidine) but not of all (e.g., carboxymethyllysine) AGEs. However, about 76% of the SAF can be explained by the variability of pentosidine.6,7
METHODS
In our study, 100 diabetic patients were included, in the implementation of cometech project. They underwent detailed history and full clinical examination. We also measured the height and body weight and calculated the body mass index (BMI), we measure the blood pressure in the arm and the patients underwent arterial duplex sonogram (Doppler examination) in the legs at the level of the ankle and calculated the ankle-branchial Index (ABI). The ABI is the ratio of systolic blood pressure measured at the ankle-at the pedis dorsalis or posterior tibial artery-divided by the systolic blood pressure measured in the arm at the brachial artery. The ABI has been presented as an important tool for diagnosing peripheral artery disease, which is a severe macrovascular complication of diabetes. The sample’s general characteristics are presented in Table 1.
| Table 1. Patients’ General Characteristics (n=100) (Mean±SD or n) |
| Men/Women (n) |
68/32 |
| Age (years) |
59.7±14 |
| BMI (kg/m2) |
28.9 ± 4.6 |
| Duration of diabetes |
19.4±12 |
| HbA1c (%) |
7.3 ± 1.4 |
| Smokers/Non-smokers |
28/72 |
| Overweight/Obese/Normal weight (n) |
36/46/18 |
| Treatment: Insulin/Oral pharmacotherapy |
32/68 |
| Education: Primary/Secondary/Tertiary (n) |
18/48/34 |
The study’s protocol was approved by the ethical committee of the International Hellenic University. Participants provided their written consent after being informed of the study’s nature and the study was conducted according to the declaration of Helsinki. All patients were ambulatory and free of acute illness.
The “continuity of care in MEtabolic diseases through modern TECHnology” (COMETECH) project, founded by Interreg IPA Cross-border Cooperation Programme “Greece-Republic of North Macedonia 2014-2020”, implements electronic medical information and communication technologies to provide and support health care in areas of Northern Greece and North Macedonia. International Hellenic University is the lead partner and Florina Prefectural General Hospital and Medical Association of Thessaloniki are participate from Greece as well as two hospitals from Republic of North Macedonia: Clinical Hospital Bitola and General Hospital Veles. The results presented here come from the International Hellenic University.
We non-invasively measured SAF, in all the participants using the AGE Reader (DiagnOptics Technologies BV, Groningen, The Netherlands). Subjects lay their arm on a special arm rest with a window in the middle (Figure 1).
Figure 1. AGE Reader (DiagnOptics, Groningen, the Netherlands). The Subject Lays his/her Forearm on the Blue Field, so that no Outside Light can Penetrate the ‘Measurement Window’
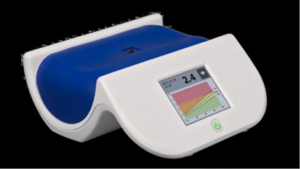
A skin surface of around 4 cm2, is illuminated with an excitation light source (maximum intensity at a wave length of approximately 370 nm) in a frequency range of 300 to 420 nm. The autofluorescent light is captured, analysed and SAF is expressed in arbitrary units (AUs). In Table 2 skin autofluorescence results in healthy adults and in type 2 diabetic patients are displayed. The results are displayed within seconds, together with age-corrected reference values.
| Table 2. Skin Autofluorescence (SAF) Measured with AGE Reader |
| Age Group (Years) |
SAF in Healthy Adults (AU) |
SAF in Type 2 Diabetes (AU) |
| 40-49 |
1.84±0.4 (n=64) |
2.17±0.5* (n=44) |
| 50-59 |
2.12±0.3 (n=199) |
2.57±0.7* (n=47) |
| 60-69 |
2.50±0.6 (n=278) |
2.69±0.7 (n=32) |
| 70-79 |
2.76±0.6 (n=307) |
3.04±0.8 (n=37) |
| >80 |
2.89±0.5 (n=108) |
3.17±0.7 (n=7) |
| Adapted from Lutgers et al11 |
Statistical Analysis
Statistical analysis was performed using statistical package for social sciences (SPSS) software (version 23, SPSS, Inc, Chicago, IL, USA). Continuous variables were displayed as means±standard deviation (SD). The associations between variables measure by Pearson’s correlation coefficient test.
RESULTS
The mean value of SAF expressed in arbitrary units (AUs) was 2.9±0.63. We examine the correlations between AGEs accumulation evaluated by SAF and hemoglobin A1C (HbA1c), blood glucose, age, gender, BMI, duration of diabetes, smoking status, blood pressure and ABI. The SAF was positive significantly correlated with age, duration of diabetes and systolic blood pressure and was negative correlated with ABI. However there was no significant correlation with heart beats, SpO2 , smoking, BMI, diastolic blood pressure, blood glucose and HbA1c (Table 3).
| Table 3. Results of correlations with SAF |
| Variable |
Pearson Correlation |
p |
| Age |
r=0.55 |
<0.05 |
| Diabetes duration |
r=0.27 |
<0.05 |
| Systolic blood pressure |
r=0.34 |
<0.05 |
| ABI |
r=-0.25 |
<0.05 |
| Heart beats |
r=-0.28 |
<0.05 |
| SpO2 |
r=-0.27 |
<0.05 |
| Smoking |
r=0.1 NS |
NS |
| HbA1c |
r=0.8 |
NS |
| Blood glucose |
r=-0.1 |
NS |
| Diastolic blood pressure |
r=0.2 |
NS |
| BMI |
r=-1.9 |
NS |
DISCUSSION
This cross-sectional study was conducted to evaluate the association between AGEs accumulation, assessed by SAF measured using the AGE Reader, and the prevalence of several metabolic variables in a diabetic population. The measurement of SAF has become a noninvasive method of assessing the accumulation of advanced glycation endproducts (AGEs) as a marker of the longterm impact of glycemic and oxidative stress in humans. In contrast to blood glucose and to HbA1c, which reflect a short period of glucose levels, the AGEs is a marker of the metabolic legacy effect and reflect a long period of glucose levels. AGE accumulation is part of the normal aging process.6 Several studies have demonstrated that calendar age is associated with increased AGE levels in humans.6
In this study the mean levels of SAF was 2.9±0.63 and was significantly correlated to age and the duration of diabetes. AGEs may reflect cumulative glycemic exposure and are less sensitive to enzymatic degradation and proteolysis. Moreover, aging may reduce the expression and activities of antioxidant enzymes, such as glyoxalase, a crucial enzyme for detoxification of methylglyoxal.6,7 AGEs may also suppress antioxidant enzyme expression and activity. Therefore, crosstalk exists between aging and AGEs; physiological aging creates numerous conditions that stimulate the accumulation of AGEs, which then accelerate the aging process in target organs.
SAF was not significantly correlated to traditional markers of glycemic control, as are blood glucose and HbA1c. These markers of glycemia reflects a very short period in contrast to AGEs, which reflect long period of glycemic control. Although HbA1c has been the gold standard for metabolic control, the DCCT/ EDIC Research Group showed that HbA1c values explained up to 11% of the risk of diabetic retinopathy, and that the unexplained 89% of variation in risk was due to elements of the diabetic milieu not captured by mean HbA1c value. The reason is that HbA1c does not reflect long-term hyperglycemia tissue expose and does not provide information about the intensity of fluctuations of blood glucose levels.
SAF was significantly correlated to high blood pressure and to peripheral arterial disease (PAD), evaluated by the ankle branchial index (ABI). This is in concordance with the results of other studies, which found SAF to be significantly higher in the PAD patients than the controls, especially in the PAD patients with cardiovascular comorbidity.8 Furthermore, SAF has been shown to be an independent predictor of amputation.9
In contrast to the results of other studies, we did not find a correlation between cigarette smoking and SAF. However, in our study we did not take into consideration the duration of smoking or the packs per year. We also did not find a correlation between BMI and SAF. However, this is in concordance with the results of van Waateringe’s study who examined the SAF and its association to components of metabolic syndrome.10 Even if there was not a significant association between BMI and SAF, however subjects with enlarged waist circumference had higher SAF, implying that not generally obesity but visceral obesity might have more impact on AGEs accumulation and SAF.
CONCLUSION
AGEs play a pivotal role in the development and progression of diabetic complications. SAF has been validated as a simple, non-invasive method for assessment of AGEs accumulation in the body. SAF is a useful clinical tool for rapid assessment of risk for AGE related peripheral artery disease, diagnosed by low ABI, which is a severe long-term macrovascular complication of diabetes. Further studies are needed to prove the value of SAF as a useful clinical tool for other microvascular and microvascular long-term diabetic complications.
FUNDING
This research was funded by Interreg Pre-Accession Assistance (IPA) Cross Border Cooperation (CBC) Programme “Greece-Republic of North Macedonia 2014-2020” co-financed by the European Union under the Instrument for Pre-Accession Assistance (IPA II). Project co-funded by the European Union and national funds of the participating countries.

CONFLICTS OF INTEREST
The authors declare that they have no conflicts of interest.







