INTRODUCTION
Tibial tubercle avulsion fractures were first described by Poncet in 1875 and were once thought to be only seen in pediatric patients.1,2 It is now accepted that adults can present with this fracture and treatment modalities for this fracture in adults include fixation with screws, sutures, and wires with either an open or arthroscopic technique.3,4 One study estimated that tibial spine avulsion fractures may be present in 14% of Anterior Cruciate Ligament (ACL) injuries. As this injury is inherently uncommon and most frequently seen in the pediatric population,5 the incidence of adult avulsion fractures may be underestimated.1
Ten case reports, including 17 patients, of ipsilateral simultaneous rupture of the patella tendon and ACL have been reported.6–16 There was one case report of a tibial tubercle avulsion fracture and a tibial spine avulsion fracture with no rupture of the patella tendon.17 This report outlines the unique situation when both of these fractures occur together with a patella tendon rupture and we provide a logical treatment option for this complex injury pattern.
CASE REPORT
The patient was a 19-year-old male who presented to the emergency department with an initial chief complaint of left knee pain. He was a college student on the intramural water polo team. On the day of his injury, the patient was riding his bicycle when he lost control and fell. He states he was riding with no hands when his left knee hit his handle bar. His leg then was caught on the ground as he attempted to plant and was internally rotated. The patient denied landing directly on the knee. Immediately after the accident he was unable to ambulate, denied any other complaints at this time, and was otherwise in excellent health, with no past medical history. On physical examination, the patient was a well-developed and muscular adult male lying comfortably in his bed with no apparent distress. Upon evaluation of his knee, there was moderate swelling and effusion present, with no evidence of an open wound. The knee was tender to gentle palpation over the lateral joint line and over the tibial tubercle and was noted to have a positive patellar ballottement. The patient’s sensation was intact to light touch distally and his pulses were 2+ and palpable. The inferior patella tendon was noted to have a large palpable defect. Despite a good effort on his part, the patient did not tolerate any range of motion to his knee. Ligamentous examination showed no evidence of medial or lateral laxity, but there was a positive Lachman despite the patient guarding. We were unable to perform a posterior drawer and the patient could not perform a straight leg raise. AnkleBrachial Index (ABI) was assessed as well and was 1.09 on the affected side (left) and 1.2 on the unaffected side (right). (Figure 1).
Figure 1: Initial radiographs obtained in the emergency room.
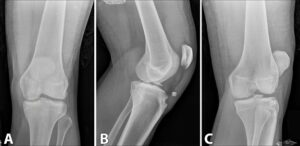
(A) AP view, (B) lateral view. Intercondylar eminence fracture and tibial tubercle avulsion shown. (C) oblique view.
A radiograph of the left knee (Figure 1) showed an osseous avulsion injury at the insertion of the patellar tendon with superior displacement of the tibial tuberosity and an accompanying patella alta. There was also a mildly displaced fracture of the lateral intercondylar eminence as well as a possible cortical disruption near the medial intercondylar eminence, plus a large effusion and anterior soft tissue swelling. The findings were suggestive of multi-ligamentous injury and were particularly concerning for ACL and Posterior Cruciate Ligament (PCL) tear equivalents. We next ordered a Magnetic Resonance Image (MRI) of the left knee, which showed a fracture at the base of the tibial eminence (Figure 2).
Figure 2: (A) and (B) demonstrate coronal views of the affected knee. Marrow contusions are apparent as well as the injuries to the medial and lateral menisci. (C) Sagittal section of the knee demonstrating the fracture to the tibial eminence and the intact PCL.
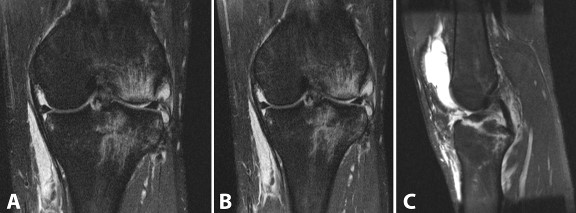
There were marrow contusions of the medial and lateral tibial plateau, lateral femoral condyle, and fibular head. The ACL was intact but had avulsed the bony fragment from the tibial eminence. The patellar tendon was intact but redundant and had avulsed a bony fragment from the tibial tubercle. There was also a complex tear of the posterior horn of the lateral meniscus and a tear of the medial meniscofemoral ligament with slight extrusion of the medial meniscus. The popliteus and soleus muscles showed grade 2 strains. A large joint effusion with lipohemarthrosis was present with a small ruptured Baker’s cyst.
At this time the all treatment options and their risks and benefits were discussed with the patient and he elected to proceed with operative treatment of his injury.
SURGICAL TECHNIQUE
We proceeded with open operative fixation and performed this one day after the injury. A standard longitudinal incision was made centered over the patella. Following this, skin flaps were created and our dissection was carried down to the frayed patellar tendon. We noted a sizeable tendon defect as well as an osseous avulsion at the tibial tuberosity insertion centrally. There was a portion of the tubercle which remained attached to the central patellar tendon proximally. As we evaluated the patellar tendon itself, we saw that the medial limb of it was partially intact with only moderate disruption of the superficial fibers. However, the lateral aspect of the tendon had been completely avulsed from the tubercle, leaving it attached to the inferior pole of the patella with a split in the coronal plane.
A large amount of hematoma was evacuated from the joint through medial parapatellar arthrotomy. The anterior cruciate ligament remained intact and attached to the avulsed tibial eminence. Provisional reduction of the bony fragment was achieved using K-wire fixation with the knee held in flexion. Final position of the fracture fragments was fixed using a 4.0 mm×38 mm partially threaded cannulated screw.
With the knee placed in extension the avulsed tibial tubercle was brought back to its native position. Placement was confirmed with k-wire fixation and a 3.5 mm×28 mm partially threaded cannulated screw held the avulsed portion of the tubercle in anatomic reduction. Once the central portion of the injured tendon was repaired we were able to repair the avulsed lateral limb of the tendon. A 4.5 mm suture anchor was placed laterally, adjacent to the tibial tuberosity, and threaded through the deep portion of the lateral tendon in a Krakow fashion. This restored the deep layer of tendinous attachment to the tibial insertion leaving to superficial sleeves of tissue both medially and laterally.
The remainder of the patellar tendon repair was done in standard fashion with a No. 5 Ethibond suture using Krakow technique in the medial and lateral tendon limbs. Beath needles were passed through the patella from distal to proximal using fluoroscopy to ensure the patellofemoral articular surface was not violated. Suture ends were passed through the patella’s inferior pole, then tensioned and sutured over the superior pole. Lastly, a drill hole was made through the center mass of the patella from medial to lateral under direct visualization. No. 5 Ethibond suture was weaved through the soft tissue proximally through the patellar tendon, circumferentially around the patella, then distally down the opposite tendon limb. This was passed through the transverse drill hole, tensioned and tied (Figure 3).
Figure 3: Intraoperative photograph showing the repair to the patellar tendon as described.
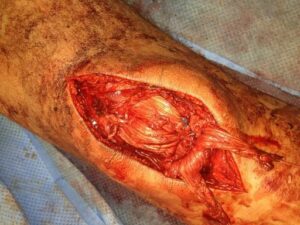
Postoperatively the knee was placed in a hinged knee brace locked in extension. The patient was allowed to be weight bearing as tolerated in this brace.
Postoperative Course
The patient was discharged from the hospital on postoperative day number 2 and followed up at regular intervals of 2 weeks (Figure 4), 6 weeks, 3 months (Figure 4), 6 months, 1 year and 2 years.
Figure 4: Radiographs during the post-operative follow-up.
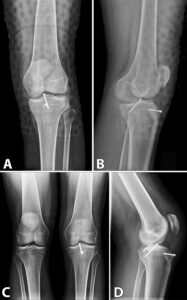
At 2 weeks, the patient had a well healing incision. He was instructed to weight-bear as tolerated with his hinged knee brace locked in full extension. We began gentle active and passive range of motion from 0-80 degrees. His X-rays showed stable hardware in good alignment. There was no evidence of bony healing at this early time.
At 6 weeks post-operatively, the patient continued to progress. He was allowed to bear weight in his hinged knee brace open to 90 degrees range of motion. At this point we initiated formal physical therapy consisting of standard quadriceps/patellar tendon repair guidelines per our physical therapy department. The X-rays obtained at this visit demonstrated evidence of bony resorption at the tibial tubercle, consistent with ongoing healing. The hardware continued to be in good alignment and showed no evidence of failure.
At the 3 months follow up visit we discontinued his hinged knee brace. There was a persistent knee effusion that was troubling the patient and we aspirated his knee at this time. There was no evidence of infection and the patient experienced relief. We obtained final follow up X-rays at this visit demonstrating that the bony fragments began to exhibit callus formation. The hardware was fully intact and in good alignment.
When the patient returned for his 6 month visit we provided a custom ACL brace for ongoing therapy as he was now ambulating around the college campus without difficulty. We elected to continue to restrict the patient’s activity and hold him from participating in water polo.
At the 8 month follow up, functional testing showed a 40-50% deficit in his quadriceps strength. He was continuing to work with focused therapy and we continued his activity restrictions. At 1 year postoperatively, the patient was doing very well. His only complaint was that he continued to experience fatigue after a short time of activity. He had been performing light activity consisting of frisbee golf, use of an elliptical trainer, and similar level activities. He had fair quadriceps tone, negative Lachman’s, and no joint line tenderness. He was able to perform a straight leg raise without lag and only exhibited a minimal amount of opening with varus stress (but still with firm endpoint). We allowed him to return to water polo at this time and insisted that he continue to work with therapy for strengthening and conditioning.
At his final appointment at 2 years postoperatively, the patient was having no issues. He had returned to full activity and participation in sports. He had no complaints and his exam was normal. He was allowed to follow up as needed in the future.
DISCUSSION
Our case report represents a unique mechanism of injury as well as a unique fracture pattern. The mechanism of injury for tibial spine avulsion fractures in adults has been described as often involving patients in motor vehicle crashes whose knee is near full extension then suddenly forced into full extension without any rotation forces.1 Tibial tubercle avulsion fractures are likely related to the intense forces generated when there is forced quadriceps contraction against a flexed knee.18 Although, our patient does not recall the precise movements of his knee, he did describe how he was riding his bicycle without any hands and attempted to plant his feet against the bicycle pedal. Unfortunately for him, his left knee missed the foot pedal and his foot landed on the ground. We surmise that the patient tried to extend his leg to push off on the pedal and forced his leg into extension against an axial load from the ground causing a tibial spine avulsion fracture. The simultaneous pull of his quadriceps muscle to attempt to extend his leg to push off the bicycle pedal caused the tibial tubercle avulsion fracture and his patella tendon rupture. The patient did also state that he felt his leg internally rotate. It is not clear how such rotation played into the fracture pattern, but may have contributed to the force needed to cause the tear of his posterior horn of the lateral meniscus.
The repair strategy for patella tendon ruptures is in general immediate open repair and several studies have outlined arthroscopic techniques to fix tibial eminence avulsion fractures in adults.19–22 Given the fact that an open repair of the patella tendon was necessary we elected to perform the repair of the tibial eminence fracture with an open technique as well. As described above, an antegrade nail was used to repair the tibial eminence fracture, which is the most effective method to obtain initial rigid fixation of the ACL avulsion fracture.22
The above case represents a unique fracture pattern as well as a unique mechanism of injury. While most tibial eminence avulsion fractures are repaired arthroscopically, this particular fracture was fixed with an open technique due to the necessary open patella tendon repair. This case may guide future surgeons in proper treatment of this very unusual case of ligamentous and bony injuries around the knee.
CONSENT
The authors affirm that the patient was told that the details of the case would be submitted for print and digital publication and provided informed consent.
CONFLICTS OF INTEREST
The authors received no funding for the study and report no conflicts of interest. David C. Flanigan is a consultant for Sanofi and Smith & Nephew.









