INTRODUCTION
Generally recurrent and metastatic cancer cervix consequences are regarded to be poor. However, some patients with limited metastasis may progress slowly. The data on oligometastatic disease in cervix is limited and hereby we present 3 cases who survived more than 5-years after developing metastasis.
CASE 1
A 40-year-old premenopausal, multiparous lady, was evaluated for intermenstrual bleeding in 2001. Per vaginum examination revealed a 1.5×1.5 cm proliferative growth in the posterior lip of cervix with free fornices, clinically Stage-IB1 disease based on the International Federation of Gynecology and Obstetrics (FIGO) staging system.
Punch biopsy from the lesion showed features of keratinising squamous cell carcinoma. Ultrasound abdomen revealed a mass lesion in the uterine cervix. She underwent radical hysterectomy with bilateral pelvic lymph node dissection. Histopathology was reported as squamous cell carcinoma of cervix infiltrating more than two-third of the thickness, with no significant pathology in the vagina, parametrium, ovaries, fallopian tubes and endometrium. Her post-operative period was uneventful and she was kept on follow-up
In 2004 she presented with complaints of lower backache. She was evaluated with a bone scan which showed increased uptake in the L3 vertebra and sacrum. There was no evidence of local recurrence. She was treated with palliative radiation 20 Gray in 5 fractions, to the lumbar spine and sacrum. She was kept on follow-up with clinical evaluation was performed every 6-months for the first 3-years and then yearly afterwards. A bone scan, performed in 2009 showed no evidence of metastasis. She is currently well and alive in 2019.
CASE 2
A 52-year-old multiparous lady was diagnosed at another centre with non-keratinising squamous cell carcinoma of cervix stage IIA in 2004. She was treated with concurrent chemoradiation, 40 gray in 20 fractions as external beam radiation to the pelvis along with concurrent cisplatin, followed by vaginal brachytherapy. She was on regular follow-up.
In 2008 she presented with complaints of persistent lower backache. She was evaluated with a computed tomography (CT) scan at our centre which showed a destructive lesion with paraspinal soft tissue component involving L5, S1 segment of the vertebral body. Multiple enlarged nodes with central hypodensity were noted in relation to the aortic bifurcation with infiltration to the right ureter and right psoas muscle causing right hydroureteronephrosis. A bone scan was performed which showed increased uptake in the L4, L5 vertebra and the upper plate of sacrum. Fine needle aspiration cytology (FNAC) from the vertebral lesion showed features of squamous cell carcinoma, suggesting metastasis from the carcinoma cervix.
She received chemotherapy (paclitaxel and cisplatin) upto 6 cycles followed by radiotherapy to para aortic nodes and lumbar spine (35 gray in 4-weeks was delivered in view of overlap with old radiotherapy fields). She is on regular follow-up with clinical examination, X-rays of the spine and abdominal ultrasound performed every six-months for the first 3-years and then yearly afterwards. She had no significant symptoms in January 2019.
CASE 3
A 55-years-old postmenpausal, multiparous lady was diagnosed with non-keratinising squamous cell carcinoma cervix, clinically stage IB. She underwent Wertheim’s hysterectomy and bilateral lymph node dissection (bilateral obturator and pelvic nodes) at another centre. Histopathology revealed squamous cell carcinoma cervix, large cell non-keratinising type with infiltration to isthmial region and bilateral lymph node metastasis.
At our centre she received adjuvant chemoradiation, 45 gray in/25 fractions as external beam radiation to the pelvis along with weekly Cisplatin 40 mg/m2 followed by two sittings of vaginal vault brachytherapy, 3 gray to point A. She was kept on regular follow-up.
In November 2005 she complained of of cough. CT chest revealed a 5×3.2 cm mass lesion in the right lower lobe. CT guided biopsy from the lesion favoured squamous cell carcinoma. There was no evidence of local recurrence. She received chemotherapy with cisplatin and 5 fluorouracil with a view to consider surgical treatment after 3 cycles of chemotherapy. But achieved complete response with chemotherapy. Post chemotherapy scans showed no evidence of disease and surgery was not done. Her chest X-rays, before and after chemotherapy are shown in Figures 1 and 2. She is on regular follow-up with clinical examination and chest X-rays performed every 6-months for the first 3- years and then yearly afterwards. She is aymptomatic since January 2019.
Figure 1. Solitary Metastasis from Carcinoma Cervix in Right Lung
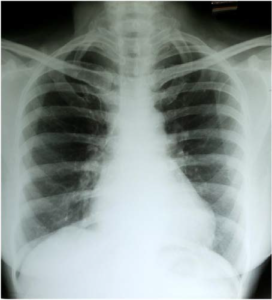
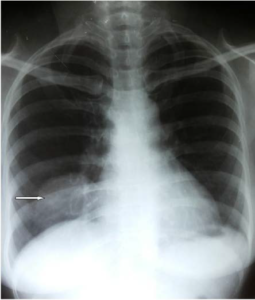
Figure 2. Complete Disappearance of Lung Lesion after Chemotherapy
DISCUSSION AND CONCLUSION
The term oligometastasis introduced in 19951 represents an intermediate state between localized disease and widespread metastasis.2 The implies is that oligometastasis can be cured with metastasis directed therapy. It is the state in which the patient shows relapse in a limited number of distant sites.3 Aggressive therapy to metastatic tumors may downsize tumor and the remaining cells may be more sensitive to chemotherapy.4 For a tumor cell to colonize a distant organ, genetic and epigenetic changes in tumor expression are required, to enable the tumor cells to overcome boundaries, survive in circulation, evade immune system, and colonize distant organs.5 Gupta and massague have framed the genes important to each of the steps of metastasis and characterized these into three categories-initiator genes, progression and virulence genes.6
Oligometastasis or oligorecurrence in distant lymph nodes have been reported in carcinoma cervix due to its spread through the lymphatic route rather than the hematogenous route.7 The first site of nodal metastasis is usually the paraaortic lymph nodes (PALN). The survival in patients with paraaortic lymph node metastases is considered to be dismal. Its incidence of detection after treatment of primary carcinoma cervix is 1.7% to 12%.8 Grigsby et al9 described the outcomes for 20 patients with PALN metastases treated between 1959 and 1986 using conventional radiotherapy with a median dose of 46.4 gray. The survival rate in this study was dismal. All patients died within 2-years after isolated PALN recurrence. Chou et al10 reported on 19 patients with isolated PALN metastases. Fourteen of the patients underwent cisplatin-based concurrent chemoradiotherapy (CCRT), 4 underwent chemotherapy alone, and 1 underwent rhabdoid tumor (RT) alone. The radiation dose was 45 gray. The 5-year overall survival (OS) rate was 31%, and asymptomatic patients who received CCRT were the only long-term survivors, with a 50% 5-year survival rate.
The frequency of intra thoracic metastasis from carcinoma cervix is approximately 10%11 while the frequency of bone metastasis from carcinoma cervix is 8.3%.12 The most frequent site of metastasis was represented by the spine (54.2%) and the pelvis (24.6%).13 Metastatic spread to the bone may occur both by direct extension of the pelvic tumour to the bone, as from soft tissue metastasis outside the pelvis, and least commonly by haematogenous route.
Many studies have reported survival outcomes of carcinoma cervix patients with paraaortic lymph node metastasis but data regarding oligometastasis to lung and skeletal system are scant.
In this case series, we have reported outcomes of a few patients with oligometastases to lungs, bone and paraaortic lymph nodes. There were no patient-related or disease-related factors which could account for the prolonged survival. There were no clinical or pathological differences between these cases and other high grade cases. It has been demonstrated that, patients with carcinoma cervix with oligometastasis have a long survival when treated with a radical intent.
CONSENT
The authors have received written informed consent from the patient.
CONFLICT OF INTEREST
The authors declare that they have no conflicts of interest







