INTRODUCTION
Microneedling is an efficient and valuable procedure that can be used to tighten, regenerate and rejuvenate the aged skin in natural way. This modality has proved it, can reverse the physical as well as histopathological signs of aging, taken into account the easiness of its application and free risk procedure with no downtime.1
Skin microneedling therapy, a physical technique, also known as collagen induction therapy or percutaneous collagen induction, is a recent addition to the treatment armamentarium for managing and combating skin aging signs.
Ageing of the skin is a multifactorial incident which mingles of the cumulative effects of chronic exposure to sun UV radiation, degradation and decline of elastin fibres, noticeable collagen reduction incurring wrinkle progress, as well as development and profound digging out.
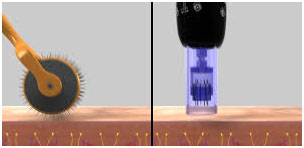
This innovative technique of microneedling is real revolutionary and considered to be a great breakthrough in microchanneling for beautification of the skin, eluding pain and no downtime. It can be carried out by a simple handy and relatively cheap modality called the 1-dermaroller (Figure 1) or a slightly costly 2-dermapen (Figure 2)-an advanced automated electrical calibrated microneedling device (fractional mechanical resurfacing), and 3-expensive comparatively the fractional controlled microtunneling laser. Both tools are however simple to employ as they are remarkable hand held medical devices which naturally increase the levels of collagen and elastin in the treated skin.
Figure 1: Derma Roller®

Figure 2: Derma Pen®

It assists in minimizing the appearance of acne and surgical scars, post-burn scar, post-traumatic scar, hypertrophic scars, varicella scars,2,3 diminishing fine lines and wrinkles, uneven skin tone and pigmentation, minimize pores, reduce sebum production, reducing skin imperfections and tightening the skin and increasing firmness, minimizing stretch marks, striae and cellulite and improving skin texture and increasing blood supply to the skin along with hydration.
Microneedling also assist in removing the scales and sebum residue around the hair infundibulum.3,4
The skin comprises a barrier to penetration of exogenous substances to the body, skin and the hair.4
The foundation of this method is to crack collagen strands that tether the acne and surgical scar to the bottom of the dermis, by microscopic-controlled injuries inflicted by the entrance of the tiny needles of the roller into the skin. This result in vascular formation and maturation, with dialation and widening in the hair infundubulum, thus ensuring neo-angiogenesis and neo-collagenesis via inducing of the natural wound-healing surge.4,5
In fact they do provide advanced micro-tunneling to the skin (skin-needling), which stimulates the skin to self regenerate and self repair naturally and safely, promoting a smoother, brighter, radiant, healthier younger-looking skin. Average 6 treatments are recommended every month to achieve desired results.
Microneedles technique had been endeavored to move and bypass across the skin in vertical, diagonal and horizontal lines on the top skin surface (stratum corneum) in order to create microchannels to the underlying epidermis and upper dermis with disrupting it. Histological studies have shown that single microneedle insertions can reach down the stratum corneum.6
THE ROLLER INVENTION
Some authors claimed that the micro-needling was first acknowledged as a potential technique in cosmetology when Andre Camirand7 noted that the scars become less visible by the technique of dry needling in 1997 by using a tattoo gun without ink to relief the surgical scars.
However, others said that the concept of micro-needling was dated back to Orentreich when he described it in subcision of scar in 1995.8 Then in 2000 a German inventor called Liebl with a plastic surgeon Fernandes suggested self designed a drum shaped device with projecting fine needles in 2006.3
THE TALE OF THE MICRONEEDLING
The microchannels created will spontaneously close after 10 minutes and the epidermal barrier integrity will remain intact.4
The principle behind microneedling lies on release of platelet derived growth factors namely transforming growth factor-alpha and beta (TGF β-3) done by micro-tunneling and puncturing the dermal vessels. Once TGF β-3 is released, they exist for around two weeks which helps in regeneration of skin by scar reduction, remodeling and improvement on the longer run.
Moreover other growth factors released are connective tissue activating protein, connective tissue growth factor, and fibroblast growth factor.3
The previous applied concept and method for treatment consisted of the use of the roller vigorously on the skin where the skin will be bleeding and oozing heavily (called vampire lift) and eventually takes longer time to recover spontaneously. However, taking into account the social shaming, need for fast recovery and to commence daily activities, wherein the patients can resume work without any need for recovery time or absenteeism, the concept slowly became less intensively used and eventually declined. Thus, puncturing the skin should not aim to ooze blood and as the target collagen is not below 0.5 mm in the upper dermis in order to induce collagen production and remodeling. Therefore, this way will aid in the building up of the level of TGF β-3 to the maximum level where the benefit will prevail.
It has been postulated that adding up a well-selected special cocktail of peptides can optimize results by specific product delivery through the tiny holes made by the dermaroller or the dermapen by increasing its permeability. Moreover these micro-needling creates temporary channels to the dermal microcirculation and induce new vessel formation, which will ultimately cause tightening of the skin along with regeneration and rejuvenation.
It is additionally important to note that many people require multiple micro-needling treatments in order to reach their desired cosmetic goals.
THE MECHANISM OF MICRONEEDLING
The foundation of microneedling is based on the concept of controlled mechanical stimulation of the wound-healing response, which is categorized into three main phases: 1-initiation of inflammation/inflammatory stage by triggering the attraction of both neutrophils and platelets in the injury site causing release of growth factors namely the TGF α and β and platelet derived growth factor which all facilitate the manufacture and dissemination of intercellular matrix proteins 2-proliferation of monocytes, keratinocytes and fibroblasts under the effect of the growth factors and thus collagen will be laid down and 3-remodeling, whereby collagen I will be formed through some process and conversions which ultimately causes skin tightening.5
However, have stipulated the actual mechanism is that the microneedling will change the cell membrane potential from resting-70 mV to 100 mV which will trigger an increase in the cell activity releasing certain mediators such as proteins, potassium, and growth factors from the cell into the surrounding intercellular matrix leading to attraction of fibroblasts to the injury area by the microneedling and thus collagen induction and synthesis happen.3
Nonetheless, reliance on ablative rejuvenation has reduced dramatically whilst non-ablative modalities emerged strongly and become an attractive alternative procedure, as they help in rejuvenation of the skin with minimal downtime and complications.9
The use of traditional ablative methods including fractional laser resurfacing and dermabrasion are, by their constitution, tremendously physically disrupting to the epidermis and upper dermal layer which all require significant prolonged healing times and all of which would trigger an inflammation and could end up on dyschromias and post-inflammatory hyperpigmentation of skin and its appendages.10
What matters in the performance of dermaroller and dermapen is the depth of performance as nowadays there is a large ongoing sale of domestic dermarollers. These domestic dermarollers vary in depth (less than 0.5 mm) from the medical ones (ranging between 0.5 mm up to 3 mm) and each has its specific application and different ways of performance in order to achieve the desired results.
DESCRIPTION OF THE SKIN ROLLER
A skin needling roller is a single use, drum like-shaped, handheld device, presterilized by gamma irradiation. On the top of the handle is a roller studded with 192 fine microneedles in eight rows in Standard one and about 540 needles in another types, 0.5-3 mm in length and 0.1-0.25 mm in diameter, comprising of fine stainless steel needles (Figure 1).11 Those fine needles are rolled on the skin back and forth in different directions to create multiple holes for about 15 times which yeilds approximately 250 holes per square cm up to the papillary dermis depending on the pressure applied.3 A single pass makes about 16 micro punctures in the stratum corneum per square cm without disrupting the epidermis drastically.3 Whereas the dermapen is like a pen, with its tip has 9-12 needles arranged in rows, with various spend vibrating stamp.3 Also there is other modality where tissue serum infusion is incorporated.
The therapeutic benefit is achieved by promoting natural collagen production and elastin in the papillary dermis, and thus creating neovascularisation and neocollagen which helps in mitigation of scars (Figure 3).11
Figure 3: Rolling in the Skin
The idea beyond this is to stimulate collagen formation, laying down, followed by reorientation after initiation of an inflammatory process in the skin. This process needs to be repeated on a regular basis.
It had been described as well as published that the roller is like a ‘miniature medieval instrument of torture’s however it has been affirmed that using the roller improves the skin appearance and makes it brighter, smoother, more suppleness, elasticity and more radiant as the skin revives and gets refreshed with a firmer texture due to thickening of the treated skin (thickened stratum spinosum).3,5
Also recently the microneedling has extended its application over the scalp for alopecia treatment and proved to be effective leading to significant scalp density.3,9 and extended to the stretch marks and gave favorable results.
COMPLICATIONS
The expected and the potential drawbacks are local irritation and some erythema of the skin following the use of the device which can last between one to two days. Some patients’ complaint of developing painful swelling for few days at the jaw angle which could be explained due to micro-tunneling and opening of the skin, where some surface skin bacteria could enter and cause that. However, a short course of antibiotic will relief it and this can be avoided by using less pressure and smaller needles over these areas.3
CONCLUSIONS
Skin microneedling is minimally invasive technique that leads to rejuvenation with regeneration of the skin along with increased collagen production and proved to be an effective aesthetic treatment that reverses the signs of photo-damaged skin. However, multiple sessions are usually needed to maintain the improvement achieved.
Different therapeutic maneuvers were advised, used and applied throughout the years to give the face a youthful appearance. However, because each person is unique, there is no one modality that can suit and is best for everyone. It should be however tailored accordingly to each client.
CONFLICTS OF INTEREST
The author declares no competing interests.
FUNDING SOURCES
None declared.








