FOLLICULITIS
Whilst the management of burn wounds continue to evolve and improve over the years, folliculitis remains one of the common sequelae in the burned patient. Folliculitis is defined as “inflammation of the hair follicles”.1,2 Hair follicles are ectodermal mesodermal structures enriched with stem cells that are complex and highly regenerative with two subtypes namely terminal hair, which is long and thick, and vellus hair, which is fine and short.3,4 The importance of hair follicles in wound healing lies in their role as a reservoir for stem cells, which proliferate and migrate to the surface in response to a new wound.5 However, in addition to a source of wound regeneration, traumatized hair follicles in the skin affected by burns can also result in painful folliculitis (Figure 1).
Figure 1. Folliculitis
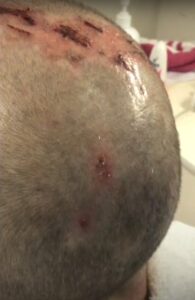
Source: The image has been screenshotted from the open source YouTube video and it is meant for eductional purpose only.17
RISK FACTORS FOR FOLLICULITIS
Patients who have sustained burns to any hair-bearing areas of the body are susceptible to the development of the often-painful complication that is folliculitis. Folliculitis can occur as early as day 3 post-burn injury and can remain an ongoing and long-term issue for burn survivors.6 Barret et al7 found that second degree burns are risk factors for the development of folliculitis but it can also occur in the setting of superficial burns.2,7,8 Additionally, it can arise on a previously healed or healing donor site from where a split skin graft has been harvested.9–12 The infection is thought to be secondary to trauma from the burn or skin graft harvest, which damage the hair follicles while also simultaneously allowing various pathogens to infect the skin.2 According to Ramirez-Blanco et al6 risk factors for developing folliculitis in burn patients include burns that involve greater than 20% of the total body surface area as well as flash burns. This may be a result of the pathophysiologic inclination in partial thickness burn where these has been damage sustained by the epidermis and the superficial dermis while preserving the hair follicle and associated adnexal elements.6 This pathophysiologic mechanism also means that the depth of debridement can also influence the development of folliculitis. Surgical debridement that removes the entire dermal layer, including the hair follicle, would theoretically minimise the risk of developing folliculitis. It has been well-documented that infections may cause skin graft failure; however, there is limited documentation regarding folliculitis as a primary cause for graft failure.13,14 It can be difficult to differentiate infection in a grafted area secondary to folliculitis compared with a true superficial graft infection. As a result, the incidence of folliculitis contributing to graft failure may be under-represented.
ORGANISM RESPONSIBLE FOR FOLLICULITIS
While maintaining a sterile burn wound environment is critical in ensuring good patient outcomes, many common nosocomial organisms remain deep-seated in the epithelial appendages including hair follicles and the sebaceous gland.15 The etiology of folliculitis can be divided into infectious and non-infectious causes, with Coagulase-Positive Streptococcus being the principal infectious pathogen found in burn patients.2,16 Other pathogens include Coagulase-Positive Staphylococcus aureus, Methicillin-Resistant Staphylococcus aureus (MRSA), Pseudomonas aeruginosa, Acinetobacter calcoaceticus sub anitratus, and Coagulase-Negative Staphylococcus.2 While rare (<10%), folliculitis can also be caused by other non-bacterial pathogens including Malassezia spp., Candida spp., herpes virus, and parasite infections.16
TYPES OF FOLLICULITIS
Folliculitis is commonly categorized according to affected body region, being divided into areas that occur on the body or areas that affect the head and neck.2 In folliculitis that develops on the body, as the early clinical presentation is that of a red spot which can progress into a pustule.2 These pustules then break open and develop crusts around the edge of the wound bed.2 The wounds are generally small, superficial, fast-spreading, and more generalized infections can recur. Folliculitis that develops in the face and scalp tend to begin as a small pustule around one or more hair follicles.2 As the pustule erupts, a crust forms that resemble impetigo without blistering.2 The wound is open with mucoid fluid covering the wound and remains inflamed while bleeding easily. If untreated, it can result in scarring alopecia.2
There are also many reported cases of head and neck folliculitis following skin graft harvest from the scalp, which is more commonly seen amongst paediatric patients where there is often a shortage of other donor sites.9–11 According to Roodbergen et al11 one way of preventing this is through harvesting a particularly thin graft, which preserves the bulge stem cell region of the hair follicles and consequently minimizes the risk of folliculitis.
DIAGNOSIS
Folliculitis is primarily a clinical diagnosis supported by qualitative findings of the organism on a wound swab.18 The use of punch biopsies has also been described to quantify the organism load, purportedly improving management decisions and overall outcomes.18 Histology samplings from punch biopsies can also confirm the presence of invasive infections.18 According to Durdu and Ilkit, the definitive diagnostic method to identify the etiology includes cytology, histopathology examinations, bacterial, fungal and/or viral culture, non-culture, and non-microscopy-based methods such as polymerase chain reaction (PCR).16 Cytology is a simple, rapid, inexpensive, and repeatable diagnostic method that can reveal various organisms that cause folliculitis.16 On histopathological examination, herpetic folliculitis demonstrates multinucleated keratinocytes, cell ballooning, intranuclear inclusion, and necrotic keratinocytes.16 While microbiological culture was once the mainstream means of determining the causing organism, PCR now provides a faster and more sensitive means of detecting these organisms.16
TREATMENT
Currently, there is no standardized pathway that identifies the best course of treatment for folliculitis in burn patients. The goals of treatment are to reduce bacterial load, promote healing and prevent complications.19 Most of the treatments focus on preventative measures and wound care with topical antiseptics, such as topical antibiotics and benzoyl.20 Other prophylactic measures include removal of hair in and around the area with a razor or clipper daily, where trimming of multiple hairs out of follicles may be required, and keeping the wound area clean with at least daily cleansing which enables removal of scabs and debris. Individual scabs should be diligently picked and removed.19
In established folliculitis, the focus is to gently debride the wound and control bacterial load with both topical antiseptic and antibacterial agents.18 Topical treatments are tailored specifically to a known pathogen. Particular therapies include; 1) fusilic acid or mupirocin ointment for Staphylococcal and Streptococcal infections, 2) dilute acetic acid bath for Pseudomonas, 3) antifungal shampoo for dermatophytes, 4) topical azoles or selenium sulphur shampoos for Pityrosporum, and 5) Permethrin cream for Demodicidosis.1 Antibiotic therapy should also be chosen according to pathogen sensitivity.1 Matheson et al2 described a treatment regimen that involves first soaking the affected area with vegetable oil to soften and remove crusts, then washing the affected area with a dilute solution of five percent chlorhexidine to aid in removal any residual debris. This regimen has been demonstrated to enable greater penetration and efficacy of the chosen topical antimicrobial therapy e.g., Povidone-iodine or silver sulfadiazine.2 Another option to enhance the efficacy of topical antimicrobial therapy involves a 15-to-30-minute soak of the affected area in a bath containing paraffin oil or five percent colloidal oatmeal, which have demonstrated good results in removing any residual crust.2
For patients with persistent folliculitis, laser hair removal is an effective treatment to prevent hair growth in the burned areas.1 Diode laser have also been shown to reduce hair density by more than 50% in all subjects 6-8-weeks after the last laser treatment.20 Other lasers that have been used include the Nd: YAG (1064 nm) and the pulsed alexandrite (755 nm).20
CONCLUSION
Despite being under-reported in the literature, folliculitis remains a source of significant burden to burn survivors. Research on folliculitis following split-thickness skin graft in burns injuries are scarce, with further studies required to identify better diagnostic and management strategies. For the clinician, it is important to be aware and remain vigilant about the potential for folliculitis, and to bear in mind preventative strategies as well as treatment to ensure the best outcomes for patients.
CONFLICTS OF INTEREST
The authors declare that they have no conflicts of interest.






