BACKGROUND AND PURPOSE
The structures of the Posterior Lateral Corner (PLC) are responsible for posterolateral stabilization of the knee. The PLC is made up of the Lateral Collateral Ligament (LCL), Popliteus Muscle Tendon (PMT), and the Popliteal Fibular Ligament (PFL). PLC injuries can be a diagnostic challenge, especially in the presence of concurrent cruciate ligament injuries, which account for 87% of all cases.1,2 Recent findings suggest that undiagnosed PLC injuries can be particularly detrimental, potentially leading to further injury of the knee. Magnetic Resonance Imaging (MRI) is considered the gold standard for diagnosing ligamentous injuries in the knee, with an accuracy of 95% for identifying major injury to the PLC structures.3 While MRI can be extremely helpful in diagnosing acute PLC injuries, they have been found to be less accurate in diagnosing chronic tears, and are costly.4 Therefore, a thorough history and physical examination should always precede MRI and guide the interpretation of diagnostic imaging results.2
A typical physical examination consists of visual observation, palpation, and range of motion, along with special testing for structural integrity. This information tells the diagnostician little about function. Currently, there is limited research on the diagnostic benefits of utilizing Functional Movement Analysis (FMA) and its role in the diagnostic process. This case report describes a false negative MRI and physical examination from two board certified orthopedic surgeons, which then required a systematic and thorough investigation of history, mechanism, and functional movement analysis by the physical therapist, leading to a non-traditional series of images to establish an accurate diagnosis.
CASE DESCRIPTION
Patient History and Systems Review
An 18-year-old Caucasian female soccer player was referred for physical therapy by an orthopedic surgeon with a diagnosis of “gait abnormality, left lower extremity.” Significant to this patient’s history is an eight-year history of Type I Diabetes and four surgeries on her contralateral right knee beginning with an Anterior Cruciate Ligament (ACL) reconstruction 2 years prior to this incident.
The patient presented to an orthopedic knee surgeon with a one-week history of left medial knee and groin pain and an abnormal acquired gait. Plain film radiographs and Magnetic Resonance Imaging (MRI) of the knee were ordered. Results were negative for bony or soft tissue abnormalities. As a result of the uncharacteristic abnormal gait pattern, lack of significant objective findings on physical examination, and negative findings on imaging studies, she was referred to another board certified orthopedic knee surgeon for a second opinion.
The second orthopedic surgeon performed a comprehensive physical examination, which included special testing for ligamentous instability. Full-length bilateral weight-bearing radiographs were ordered to assess bony mal-alignment as a possible cause for the abnormal gait pattern. These films were negative for pathology. Strength, Range of Motion (ROM), and special testing for ligamentous instability and meniscal injury were all unremarkable. Due to the uncommon gait presentation, along with negative findings on MRI and radiograph, the orthopedic surgeon suspected a neurologic lesion such as Multiple Sclerosis (MS) or peripheral neuropathy. She was referred to Neurology for an Electromyographic (EMG) study of bilateral lower extremities to rule out peripheral neuropathy. MRI studies of the cervical spine to the sacrum were ordered to evaluate for cord lesions. MRI of the brain was ordered to rule out brain lesions. MRI of the hip was also ordered to rule out intra-articular hip pathology as she was complaining of medial hip pain. Before all imaging and diagnostic studies were completed, the patient was referred to and evaluated by the physical therapist. A chronological history of events following the injury are detailed in Table 1.
Table 1. Chronological History of Events after Injury
| Week 1 |
- Visits orthopedic surgeon #1
- (-) Knee radiographs and magnetic resonance imaging (MRI)
- Referred to orthopedic surgeon #2
|
| Week 2 |
- Visits orthopedic surgeon #2
- (-) Radiographs
- Bilateral lower extremity electromyography (EMG) study ordered
- MRI of cervical spine (C/S), thoracic spine (T/S), lumbar spine (L/S), and sacral spine ordered
- Physical therapy referral given
|
| Week 3-4 |
- (-) Bilateral lower extremity EMG study ordered
- (-) MRI of C/S, T/S, L/S, and sacrum
- Brain and hip MRI ordered
|
| Week 5 |
- Patient evaluated by physical therapist
- Treating physical therapist suggests stress radiographs be taken to rule out lateral collateral ligament (LCL) strain
- (-) Brain MRI
|
| Week 6 |
- (+) Stress radiographs bilaterally for increased varus gapping
|
| 3 months |
- Arthroscopic reconstruction of LCL, posterior fibular ligament and posterior corner
|
Examination
The initial evaluation was approximately five weeks after the patient’s injury. A thorough subjective history was collected from the patient, including all events surrounding the current injury, as well as a detailed past medical history (Table 2).
Table 2. Past Medical History
| Gestation |
Cyst in utero, resolved spontaneously |
| 2 years |
Fractured clavicle, fell off bench |
| 9 years |
Running backwards, fractured wrist |
| 10 years |
Diagnosed with diabetes type 1 (insulin pump) |
| 15 years |
Fractured big toe playing soccer |
| 16 years |
Nov 2009 anterior cruciate ligament and meniscus surgery |
| 17 years |
June 2010 scar tissue debridement |
| 18 years |
Dec 2010 scar tissue debridement and anterior cruciate ligament debridement, Jan 2011 developed reflex sympathetic dystrophy, had negative bone scan, had nerve block with no relief |
| 18 years |
Feb 2011 Endo button removal and scar tissue debridement |
| 18 years |
April 7, 2011 doing kickboxing video, kicked high in air, felt awkward, then planted and felt immediate pain, next day felt laxity, and walking digressed. |
The initial mechanism of injury occurred when the patient was performing an exercise-video kickboxing regimen that called for her to do a high lateral kick in the air with her left lower extremity followed by a lateral lunge with the same extremity. She felt an awkward and unfamiliar sensation on the left lateral knee during the kick. Upon landing in a lateral lunge position with the left hip and knee flexed, she felt an immediate sharp pain in her knee. The patient recalled having a slight feeling of instability in the knee joint when walking the next day. There was a slow increase of perceived instability in the subsequent five weeks, which developed into medial knee pain and medial hip and groin pain. The patient’s self-reported outcome measure score on intake for the Lower Extremity Functional Scale was a 13/80 with an 80/80 being no disability.5
Significant past medical history included insulin dependent Type I Diabetes. Also of note was her right knee surgical history. Approximately 2 years prior to her current injury, she tore her right Anterior Cruciate Ligament (ACL) and meniscus. She had surgery to reconstruct the ligament and debride the meniscus. Six months post-repair, scar tissue debridement and release was performed secondary to knee arthrofibrosis and significant pain.6 Due to ongoing stiffness and pain she had a second arthroscopic release. She subsequently developed reflex sympathetic dystrophy six months later. She received a bone scan, which was negative for fracture, infection, and malignancy. She underwent femoral nerve block with no relief. Her retained hardware for her ACL reconstruction (Endobutton, Smith & Nephew, Andover, MA, USA) was removed and scar tissue was debrided again the following month. This was two months prior to the current injury. With injuries and surgery taking place on the right knee, the differential diagnosis process was complicated by eliminating the reference limb, which a physical therapist would typically use for side-to-side comparisons.7
Following the subjective history, a detailed gait analysis was performed (see http://openventio.org/Volume1_Issue2/SEMOJ-1-108/videos.php For online video links). At initial contact/loading response with the involved limb, the patient landed with heel strike, and did not achieve the normal 5-15 degrees of knee flexion used for shock absorption. During mid-stance, the knee collapsed to approximately 35 degrees of flexion. During the collapse there was a rapid frontal plane deviation of a varus thrust which quickly reversed into a valgus thrust with associated femoral internal rotation and adduction. There was no heel-off in terminal stance.
With the data gathered up to this point, preliminary hypotheses pertaining to pathoanatomic diagnoses were formulated, leading to a standardized gait analysis (Table 3).
Table 3. Detailed Gait Analysis
| Initial Contact Loading Response |
Demonstrates decreased knee flexion for shock absorption. The knee then collapses and there is a rapid frontal plane deviation of femoral abduction which quickly reverses itself into femoral adduction and internal rotation. |
| Mid-stance |
Full knee extension is not achieved. The femur remains in internal rotation and adduction. |
| Terminal stance |
No heel-off. |
| Swing Phases |
No significant findings. |
| Toe-walking |
Able to lock out knee without noticeable impairments. |
| Heel-walking |
Able to lock out knee without noticeable impairments. |
| Lateral side-stepping |
A feeling of instability is reported on the lateral portion of her knee when she is side-stepping toward the left. No instability noted during side-stepping to the right. |
| Backwards walking |
Demonstrates backwards walking without significant deviation. The patient is able to go from toe to heel, but does not get into full knee extension. Stride length is shortened on the left versus the right. |
The patient may have been avoiding the 15 degrees of knee flexion used for shock absorption during loading response in order to avoid the compressive forces at the patella associated with quadriceps contraction.8,9 A meniscal tear could cause the tibiofemoral joint to lock in extension during swing.9 A meniscal tear could also lead to decreased joint congruency, which decreases stability.10 Ligamentous laxity or a tear would also lead to decreased stability of the joint.9 A common compensation to improve joint stability is to fully extend the knee. Locking the knee in full extension makes the joint more stable by increasing joint congruency. Also, using an active contraction of the quadriceps and hamstrings will increase compression of the tibiofemoral joint, which increases the joint’s surface friction and makes any movement in the joint more difficult.9 Full extension also allows the posterior capsule to provide posterior stability while keeping the knee joint away from the flexion torque that is present as soon as the knee becomes even slightly flexed.8,9 The valgus thrust and collapse of the knee into 35 degrees of flexion could have been secondary to pain mediated weakness of gluteus medius, maximus and/or the quadriceps. The valgus thrust seen in mid-stance may have been an over-compensatory response to avoid feeling lateral instability following the initial varus thrust.9
Following a standard gait analysis, further functional movement analysis was used to accentuate body structure impairments. Lateral stepping to the left reproduced a feeling of instability, but was not reproduced in lateral stepping to the right. Toe-walking and heel-walking was performed in full knee extension without significant impairment or deviation of the knee in the frontal plane. The patient did not demonstrate any significant deviations or symptom reproduction during backward walking. She was able to transfer her weight from toe to heel, but did not achieve full knee extension. She also demonstrated a shorter stride length on the left versus the right. The patient was able to balance for greater than 30 seconds on a single limb, bilaterally. The patient did, however, demonstrate left lateral knee instability in static standing; while in static standing the patient swayed her knees side to side, and demonstrated a larger-than-normal varus angulation and excursion to the left, which was significantly greater than the right. The patient had associated feeling of awkward sensitivity and instability.
Considering the patient’s story, location of pain and findings from the FMA, a rupture or insufficiency of the lateral collateral ligament complex and Posterolateral corner (PLC) was suspected. Patients with neurologic pathology commonly present with motor control impairments affecting balance, backwards walking and gait. This patient was able to demonstrate most of these functional movements without difficulty, ruling down the likelihood of neurologic pathology.11,12,13 However, pathologies such as multiple sclerosis, demyelinating polyneuropathy or any pathology that could affect joint proprioception could not be ruled out before a formal assessment of the peripheral and central nervous system. With the data gathered during the FMA, the therapist proceeded with an objective table examination to rule up or down the most likely diagnoses on the differential diagnosis list.
Babinski and Hoffman’s were normal and patellar and Achilles reflexes were 2+ bilaterally. Knee active and passive ROM was approximately 0-135º bilaterally. Strength testing revealed deficits on the left for knee flexion, and hip flexion, extension, and abduction. There was associated pain with hip and knee flexion. See Table 4 for a full overview of strength testing results.
Table 4. Manual Muscle Test Grades at Initial Evaluation
|
Muscle
|
Right
|
Left
|
| Hip Flexion |
5
|
4+*
|
| Knee extension |
5
|
5
|
| Knee flexion |
5
|
4*
|
| Dorsiflexion |
5
|
5
|
| Great toe extension |
5
|
5
|
| Plantar flexion |
5
|
5 (25 heel raises with knee locked)
|
| Side-lying hip abduction |
4+
|
4-
|
| Hip extension |
4+
|
4
|
| *denotes pain |
Knee special tests revealed positive laxity with apprehension and an audible click with Varus Stress Testing on the left.14 The Dial-Test, which tests for PLC, with or without concurrent PCL injury, was positive at 30 degrees of flexion and negative at 90 degrees of flexion. This is indicative of a PLC injury without PCL involvement.15,16 Also noted was increased laxity but solid end-feel with Anterior Drawer and Lachman’s on the left.17,18,19 Pivot-shift, McMurray’s, Apley’s Compression, Thessaly’s and Valgus Stress Testing were negative.17,18,19,,20
Hip special tests were then performed. The FABER test revealed a distance of 13 cm lateral patella to the table on left versus 8 cm on the right.21 This finding can be indicative of decreased muscle length in a number of different muscles that flex, adduct and/or internally rotate the femur. It can also indicate decreased anterior hip capsule mobility.22 This test, however, is not considered positive for intra-articular pathology without the presence of pain.21 FADIR, which places the hip in end range flexion, adduction and internal rotation, and a hip scour test were both negative, ruling down the likelihood of an ace tabular labral tear.21,23 See Table 5 for a full overview of special testing findings for the left knee and hip.
Table 5. Special Testing
| Special Tests for the Knee |
| Varus Stress |
+*
|
| Dial Test |
+
|
| Varus Stress |
–
|
| Anterior Drawer |
– (2+ laxity, but solid end feel noted)
|
| Lachman’s |
– (2+ laxity, but solid end feel noted)
|
| Pivot Shift |
–
|
| McMurray’s |
–
|
| Apley’s Compression |
–
|
| Thessaly’s |
–
|
| Special Tests for the Hip |
| FABER |
– (negative for pain, but mobility/flexibility deficit note)
|
| FADIR |
–
|
| Hip Scour |
–
|
| *denotes pain |
Following the physical therapy evaluation, the therapist felt confident that lateral instability was causing the abnormal gait pattern. The varus to valgus thrust seen in mid-stance was postulated to be a protective compensation to limit varus force to the lateral structures of the knee. The medial hip and knee pain were a direct result of the compensatory abnormal gait pattern. Other major physical examination findings that supported this hypothesis included the following: a mechanism of injury that was caused by a lateral force to the knee, no apparent abnormality in toe/heel/backwards walking, normal neurologic reflexes, and a positive Dial and a positive Varus-Stress Test.
With the provisional hypothesis of knee lateral instability, and considering negative findings of ligamentous injury on MRI, the physical therapist recommended stress radiographs be performed to rule out capsuloligamentous insufficiency, and referred the patient back to the orthopedic surgeon for stress radiographs. Stress radiographs are not typically ordered in standard orthopedic practice. Radiographs with varus and valgus stress were completed. Varus stress radiographs demonstrated excessive lateral joint-line gapping, both in the knee extended and knee flexed positions. These findings confirmed the physical therapist’s hypothesis of lateral ligamentous insufficiency.24,25 The patient opted to undergo surgery to repair and augment with reconstruction of the lateral structures contributing to the structural instability (Figure 1).
Figure 1. Stress Radiographs Left Knee
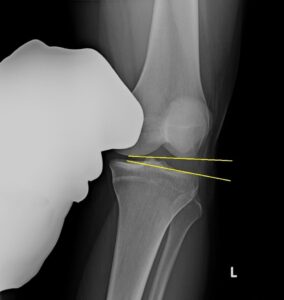
Radiograph with varus stress applied in knee flexion, revealing lateral joint line laxity.
Intervention
In preparation for surgery, the patient was seen for two pre-operative visits by the physical therapist. Treatment focused on proximal hip and knee strengthening and neuromuscular reeducation to control frontal plan deviations during the loading response and mid-stance phases of gait, and ultimately to correct her compensatory abnormal gait pattern. Treatment was also aided by the use of a SERF strap, which is a flexible strap designed to help stabilize the femur in external rotation during dynamic activities.26 This strap has been shown to control excessive femoral internal rotation as well as increase the muscular activation of the gluteus medius.
Intraoperatively, the surgeon discovered excessive laxity of both the Lateral Collateral Ligament (LCL) and the PLC, or more specifically, the Popliteal Fibular Ligament (PFL) and popliteus tendon. These ligaments along with the posterior capsule were described as being “patulous” or frayed. The LCL, PFL and popliteus tendon were reconstructed using allografts and were then sutured to the patient’s native LCL, PFL and popliteus tendon. The post-surgery protocol called for strict nonweight bearing for six weeks to minimize load on the LCL. Postoperative physical therapy was started after four weeks after surgery. The patient underwent physical therapy for six months, and returned to running without restrictions. Post-operative physical therapy consisted of active and passive range of motion, neuromuscular re-education, both open and closed kinetic-chain strengthening, and functional movement training to return the patient to a high level of exercise and running.
DISCUSSION
The patient’s gait demonstrated an abnormal varus thrust during loading response that was not seen on the contralateral limb. This was immediately followed by valgus collapse during the mid-stance phase of gait. This gait deviation may indicate that the lateral knee structures, specifically the LCL, could be compromised. Injury to the LCL is the least common of all knee ligament injuries with an incidence of 4%. Injury to the LCL usually occurs as a soft-tissue avulsion off the proximal attachment on the femur or as a bone avulsion associated with an arcuate fracture of the fibular head.3,27 LCL injuries usually are part of more extensive injuries that involve the PLC.27 The LCL attaches to the femur approximately equidistant from the posterior and distal borders of the lateral femoral condyle and distally to a superior and laterally facing V-shaped plateau on the head of the fibula.28 It is the main structure responsible for resisting varus stress, particularly in the initial 0° to 30° of knee flexion, and limits external rotation of a flexed knee.29,30
Posterolateral corner injuries account for 16% of all knee ligament injuries and often occur in combination with other ligament injuries.31,32,33 Most common mechanisms of injury include: a blow to the anteromedial aspect of the knee when the joint is in or near full extension; contact and noncontact hyperextension injuries; a valgus contact force applied to a flexed knee; or extreme tibial external rotation with the knee in flexion or hyperextension.30,31 The three most important stabilizing structures of the posterolateral knee are the PFL, popliteus tendon, and fibular collateral ligament.34 Their main role is to prevent excessive knee varus, tibial external rotation and posterolateral rotation.35,36 Though it is unclear from the description of the original injury, this patient may have injured her PLC, PFL and popliteus tendon with a similar knee varus and tibial external rotation overload, either from the lateral kick or the lateral lunge. Patients who have suffered an injury to their posterolateral corner commonly present with altered gait mechanics, however a recognizable pattern has not yet been reported. In this and other clinicians’ experiences, a varus force at the knee can commonly be seen during the loading response to mid-stance phases of gait.3 The patient may then fully contract the quadriceps to lock out the knee in hyperextension in order to create additional stability through the passive intact posterior knee structures and compression of the tibiofemoral joint.30 As seen with the patient presented in this case study, it is also possible that they will overcorrect a varus thrust using a compensatory valgus thrust during the phases of loading response to mid-stance. This pattern allows for support by medial passive and active structures such as the medial collateral ligament, semimembranosus, semitendinosus, sartorius and gracilis.30
It is important to note that while a standard physical examination with special testing for structural integrity is vital to the evaluation process; functional movement analysis can significantly affect the differential diagnosis. In this case study, the functional movement and gait analysis helped guide the clinician to request appropriate imaging and ultimately lead to a correct diagnosis, which was confirmed intraoperatively.37,38,39
CONCLUSION
In this case study, a very systematic approach to col lecting subjective information led to functional movement tests and table examination that revealed findings contrary to the orthopedists’ impression and imaging results. These findings were used to help guide clinical reasoning and ultimately confirm the hypothesis of lateral instability. While there is more discussion about the use of functional movement analysis, the literature is sparse defining how and when it should be implemented. It is a powerful and unique tool physical therapists can use in evaluating and treating patients. The findings should always be correlated with subjective information, objective tests and measures, and be confirmed by imaging when possible. More research should be done to demonstrate the role of functional movement analysis, and how it can best be implemented to determine a patient’s diagnosis and treatment plan.
ACKNOWLEDGEMENTS
A special thank you to Dr. Kornelia Kulig, PT, PhD, FAPTA, FFAAOMPT for her initial guidance with this manuscript.
CONFLICTS OF INTEREST
The authors certify that they have no affiliations with or financial involvement in any organization or entity with a direct financial interest in the subject matter or materials discussed in the manuscript.
CONSENT
For the videos shown in the practise, we have obtained the consent statement from the girl who was involved in this case study.






