Diabetes pedigree function (DPF) predicts diabetes risk based on age and family history, regardless of whether the person is diabetic or not. There is little proof to support the notion that type 2 diabetes (T2D) is a hereditary condition. In real life, it is common for a T2D patient to have T2Ds in one or more family members, such as at least one parent or sibling.1,2 Additionally, it is observed that a subject’s chance of having T2Ds rises in proportion to the number of members of his or her family who have the disease.3,4 Clinical family history of diabetes has been recognized as a T2D risk factor and provides genuine genomic data that identifies the interactions between genetic, behavioral, and environmental factors.2,3 To the best of our knowledge, there has been minimal research done on the factors that influence DPF. It is intriguing to investigate how age, body mass index (BMI), subject type (ST), such as diabetic (=2) or non-diabetic (=1), etc., relate to DPF and diabetes biomarkers. It provides some thoughts on the viability of DPF. The following inquiries are examined in this editorial note: Is there a connection between DPF and diabetes biomarkers, in addition to age, BMI, and subject type? What kind of relationship exists if the answer is yes? What functions do the explanatory factors play in the DPF? According to the results of the current study, mean DPF has a positive relationship with ST (p=0.001), subject age (p=0.033), insulin level (p=0.003), triceps skin-fold thickness (TST) (p=0.008), and joint effects of glucose level and body mass index (Glucose×BMI) (p=0.062), while it has a negative relationship with glucose level (p=0.072) and the number of pregnancies (p=0.021). A genuine data set of 768 girls of Pima Indian descent who are at least 21-years-old is used to analyze the aforementioned questions in this article. Women with gestational diabetes mellitus (GDM) and non-diabetic women are both included in this data collection. GDM typically manifests during pregnancy, when blood glucose levels are greater. The UCI Machine Learning Repository has this data collection. Age (in years), ST, diastolic blood pressure (DBP) (mm Hg), TST (mm), 2-hour serum insulin (µU/ml), number of pregnancies, BMI, plasma glucose concentration over 2-hours in an oral glucose tolerance test (Glucose), and DPF are the nine variables/factors. Based on the DPF model and the other explanatory variables/factors, the aforementioned questions can be investigated. DPF should be taken into consideration as a heteroscedastic response variable that can be represented by joint generalized linear models (JGLMs).5 The DPF model used here is based on gamma JGLMs. The DPF JGLMs are listed below: JGL gamma fitted DPF mean (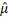 ) model is
) model is 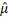 =exp(-0.447-0.018 Pregnancy Nos.-0.006 Glucose+0.004 TST+0.001 Insulin-0.019 BMI+0.0001 Glucose×BMI+0.005 Age+0.193 ST), and the JGL gamma fitted DPF dispersion (
=exp(-0.447-0.018 Pregnancy Nos.-0.006 Glucose+0.004 TST+0.001 Insulin-0.019 BMI+0.0001 Glucose×BMI+0.005 Age+0.193 ST), and the JGL gamma fitted DPF dispersion (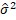 ) model is
) model is 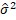 =exp(-0.788-0.090 Pregnancy Nos.-0.002 DBP+0.001 Pregnancy Nos.×Glucose). These can be derived from the DPF mean model. The ST and mean DPF are positively correlated, indicating that diabetes people have higher DPF scores than non-diabetic subjects. It demonstrates how DPF exhibits its own genesis. Age of the participant is positively correlated with mean DPF (p=0.033), suggesting that DPF score rises with age. It also meets DPF’s requirement for originality. The mean DPF is inversely correlated with the glucose level (p=0.072), indicating that the DPF score declines with increasing glucose levels. It goes against the notion that DPF and ST are positively correlated. This is as a result of the calculation not taking the glucose level into account. The insulin level and mean DPF are positively correlated (p=0.003), meaning that the DPF score rises as the insulin level does. This demonstrates that the level of insulin rises naturally as the subject’s level of diabetes increases. The TST and mean DPF are positively correlated (p=0.008), suggesting that the DPF score rises as the TST does. The mean DPF is negatively correlated with the number of pregnancies (p=0.021), suggesting that the DPF score increases as the number of pregnancies reduces. The joint interaction effect of Glucose×BMI is favorably correlated with Mean DPF (p=0.062). Stating that the combination effect of Glucose×BMI causes a rise in DPF score. Many of the above-mentioned real occurrences are confirmed by the most recent reported outcomes. To the best of our knowledge, the Editorial report contains every new finding in the literature on gestational diabetes. There are no earlier papers that can be compared to the results that were just given, so they cannot be. There are numerous associations of the variance of DPF, which will be explored in our forthcoming paper, but the editorial note just briefly discusses the mean connections of DPF. The aforementioned findings are based on a gamma fit of the DPF using JGLM, and the fitting was verified using model checking charts. Additionally, the model with the lowest Akaike information criterion (AIC=9.082) is chosen as the best model. A complex link between DPF and the remaining explanatory factors and variables has been demonstrated in the editorial note. Pregnant women, diabetes professionals, and researchers will all benefit from this editorial statement. Pregnant women are encouraged to monitor their PDF, glucose and insulin levels, BMI and TST on a regular basis.
=exp(-0.788-0.090 Pregnancy Nos.-0.002 DBP+0.001 Pregnancy Nos.×Glucose). These can be derived from the DPF mean model. The ST and mean DPF are positively correlated, indicating that diabetes people have higher DPF scores than non-diabetic subjects. It demonstrates how DPF exhibits its own genesis. Age of the participant is positively correlated with mean DPF (p=0.033), suggesting that DPF score rises with age. It also meets DPF’s requirement for originality. The mean DPF is inversely correlated with the glucose level (p=0.072), indicating that the DPF score declines with increasing glucose levels. It goes against the notion that DPF and ST are positively correlated. This is as a result of the calculation not taking the glucose level into account. The insulin level and mean DPF are positively correlated (p=0.003), meaning that the DPF score rises as the insulin level does. This demonstrates that the level of insulin rises naturally as the subject’s level of diabetes increases. The TST and mean DPF are positively correlated (p=0.008), suggesting that the DPF score rises as the TST does. The mean DPF is negatively correlated with the number of pregnancies (p=0.021), suggesting that the DPF score increases as the number of pregnancies reduces. The joint interaction effect of Glucose×BMI is favorably correlated with Mean DPF (p=0.062). Stating that the combination effect of Glucose×BMI causes a rise in DPF score. Many of the above-mentioned real occurrences are confirmed by the most recent reported outcomes. To the best of our knowledge, the Editorial report contains every new finding in the literature on gestational diabetes. There are no earlier papers that can be compared to the results that were just given, so they cannot be. There are numerous associations of the variance of DPF, which will be explored in our forthcoming paper, but the editorial note just briefly discusses the mean connections of DPF. The aforementioned findings are based on a gamma fit of the DPF using JGLM, and the fitting was verified using model checking charts. Additionally, the model with the lowest Akaike information criterion (AIC=9.082) is chosen as the best model. A complex link between DPF and the remaining explanatory factors and variables has been demonstrated in the editorial note. Pregnant women, diabetes professionals, and researchers will all benefit from this editorial statement. Pregnant women are encouraged to monitor their PDF, glucose and insulin levels, BMI and TST on a regular basis.
ACKNOWLEDGEMENT
The authors are very much indebted to the referees who have provided valuable comments and editions to improve this paper.
CONFLICTS OF INTEREST
The authors declare that they have no conflicts of interest.





