1. Walker AL, DeFrancesco TC, Bonagura JD, et al. Association of diet with clinical outcomes in dogs with dilated cardiomyopathy and congestive heart failure. J Vet Cardiol. 2022; 40: 99-109. doi: 10.1016/j.jvc.2021.02.001
2. Smith CE, Parnell LD, Lai C-Q, Rush JE, Freeman LM. Investigation of diets associated with dilated cardiomyopathy in dogs using foodomics analysis. Scientific Reports. 2021; 11: 15881. doi: 10.1038/s41598-021-94464-2
3. McCauley SR, Clark SD, Quest BW, Streeter RM, Oxford EM. Review of canine dilated cardiomyopathy in the wake of diet-associat ed concerns. J Anim Sci. 2020; 98: skaa155. doi: 10.1093/jas/skaa155
4. Dutton E, López-Alvarez J. An update on canine cardiomyopathies -is it all in the genes? J Small Anim Pract. 2018. doi: 10.1111/jsap.12841
5. Bakke AM, Wood J, Salt C, et al. Correction: Responses in randomised groups of healthy, adult Labrador retrievers fed grain-free diets with high legume inclusion for 30 days display commonalities with dogs with suspected dilated cardiomyopathy. BMC Vet Res. 2022; 18: 185.
doi: 10.1186/s12917-022-03291-8
6. Kaplan JL, Stern JA, Fascetti AJ, et al. Taurine deficiency and dilated cardiomyopathy in golden retrievers fed commercial diets. PLoS One. 2018; 13: e0209112. doi: 10.1371/journal.pone.0209112
7. Burns KM. Grain-Free Diets and Dilated Cardiomyopathy. https://todaysveterinarynurse.com/nutrition/grain-free-diets-and-dilated-cardiomyopathy/. Accessed January 25, 2023.
8. Lichtenberger J. Grain-free diets and dilated cardiomyopathy, an emerging problem? Paper presented at: the 2019 OVMA (Ontario Veterinary Medical Association) Conference; January 31, 2019 to February 2, 2019; Toronto, Canada. 118-120.
9. Gaar-Humphreys KR, Spanjersberg TC, Santarelli G, et al. Genetic basis of dilated cardiomyopathy in dogs and its potential as a bidirectional model. Animals (Basel). 2022; 12: 1679. doi: 10.3390/ani12131679
10. Freeman LM, Stern JA, Fries R, Adin DB, Rush JE. Diet-associated dilated cardiomyopathy in dogs: what do we know? J Am Vet Med Assoc. 2018; 253: 1390-1394. doi: 10.2460/javma.253.11.1390
11. Vollmar A. The prevalence of cardiomyopathy in the Irish wolfhound: A clinical study of 500 dogs. J Am Anim Hosp Assoc. 2000; 36: 125-132.
doi: 10.5326/15473317-36-2-125
12. Saito T, Suzuki R, Yuchi Y, Yasumura Y, Teshima T, Matsumoto H, Koyama H. A case of a small-breed dog with diet-related dilated cardiomyopathy showing marked improvements in cardiac morphology and function after dietary modification. Vet Sci. 2022; 9: 593.
doi: 10.3390/vetsci9110593
13. Adin D, Freeman L, Stepien R, et al. Effect of type of diet on blood and plasma taurine concentrations, cardiac biomarkers, and echocardiograms in 4 dog breeds. J Vet Inter Med. 2021; 35: 771-779. doi: 10.1111/jvim.16075
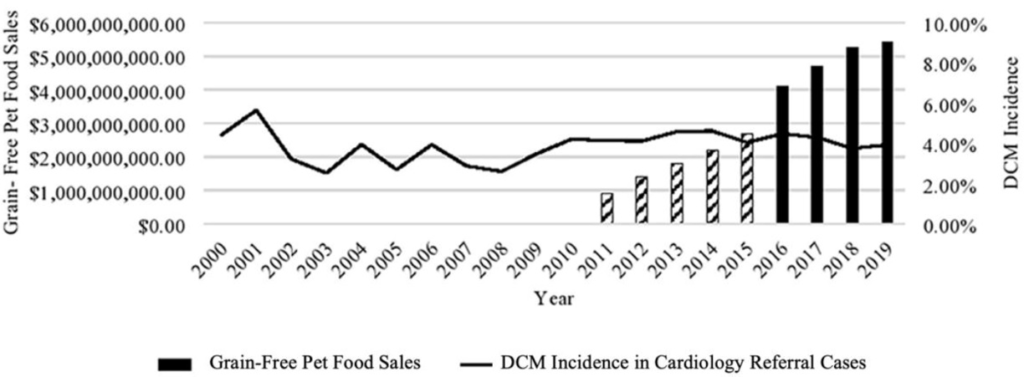
14. Quest BW, Clark SD, Garimella S, Konie A, Leach SB, Oxford EM. Incidence of canine dilated cardiomyopathy, breed and age distributions, and grain-free diet sales in the United States from 2000-2019: A retrospective survey. Front Anim Sci. 2020; 3. doi: 10.1101/2020.09.27.315770
15. U. S. Food and Drug Administration (FDA). Investigation into Potential Link between Certain Diets and Canine Dilated Cardiomyopathy. https://www.fda.gov/animal-veterinary/outbreaks-and-advisories/fda-investigation-potential-link-between-certain-diets-and-canine-dilated-cardiomyopathy. Accessed January 25, 2023.
16. Bellumori TP, Famula TR, Bannasch DL, Belanger JM, Oberbauer AM. Prevalence of inherited disorders among mixed-breed and purebred dogs: 27,254 cases (1995-2010). J Am Vet Med Assoc. 2013; 242: 1549-1555. doi: 10.2460/javma.242.11.1549
17. Fioretti M, Delli C. Epidemiological survey of dilatative cardiomyopathy in dogs. Veterinaria. 1988; 2: 1.
18. Dukes-McEwan J, Borgarelli M, Tidholm A, Vollmar AC, Häggström J. Proposed guidelines for the diagnosis of canine idiopathic dilated cardiomyopathy. J Vet Cardiol. 2003; 5: 7-19. doi: 10.1016/s1760-2734(06)70047-9
19. Smith CE, Parnell LD, Lai CQ, et al. Metabolomic profiling in dogs with dilated cardiomyopathy eating non-traditional or traditional diets and in healthy controls. Sci Rep. 2022; 12: 22585. doi: 10.1038/s41598-022-26322-8
20. Koch J, Pedersen HD, Jensen AL, Flagstad A. M-mode echocardiographic diagnosis of dilated cardiomyopathy in giant breed dogs. Zentralbl Veterinarmed A. 1996; 43: 297-304. doi: 10.1111/j.1439-0442.1996.tb00456.x
21. Wess G. Screening for dilated cardiomyopathy in dogs. J Vet Cardiol. 2022; 40: 51-68. doi: 10.1016/j.jvc.2021.09.004
22. Ward J, Ware W, Viall A. Association between atrial fibrillation and right-sided manifestations of congestive heart failure in dogs with degenerative mitral valve disease or dilated cardiomyopathy. J Vet Cardiol. 2019; 21: 18-27. doi: 10.1016/j.jvc.2018.10.006
23. Tidholm A, Jönsson L. Histologic characterization of canine dilated cardiomyopathy. Vet Pathol. 2005; 42: 1-8. doi: 10.1354/vp.42-1-1
24. Guglielmini C. Cardiovascular diseases in the ageing dog: Diagnostic and therapeutic problems. Vet Res Commun. 2003; 27: 555-560.
doi: 10.1023/b:verc.0000014216.73396.f6
25. Thomas DE, Wheeler R, Yousef ZR, Masani ND. The role of echocardiography in guiding management in dilated cardiomyopathy. Eur J Echocardiogr. 2009; 10: iii15-iii21. doi: 10.1093/ejechocard/jep158
26. Schober K, Hart T, Stern JA, et al. Detection of congestive heart failure in dogs by Doppler echocardiography. J Vet Intern Med. 2010; 24: 1358-1368. doi: 10.1111/j.1939-1676.2010.0592.x
27. Petrie J-P. Practical application of holter monitoring in dogs and cats. Clin Tech Small Anim Pract. 2005; 20(3): 173-181.
doi: 10.1053/j.ctsap.2005.05.006
28. Martin MWS, Stafford Johnson MJ, Celona B. Canine dilated cardiomyopathy: A retrospective study of signalment, presentation and clinical findings in 369 cases. J Small Anim Pract. 2009; 50: 23-29. doi: 10.1111/j.1748-5827.2008.00659.x
29. Bonagura JD, Visser LC. Echocardiographic assessment of dilated cardiomyopathy in dogs. J Vet Cardiol. 2022; 40: 15-50.
doi: 10.1016/j.jvc.2021.08.004
30. Morgan RV. Handbook of Small Animal Practice. 3rd ed. Philadelphia, USA: Saunders; 1997.
31. Singletary, G.E, Morris, N.A, Lynne O’Sullivan, M, Gordon, S.G, Oyama, M.A. Prospective evaluation of NT-proBNP assay to detect occult dilated cardiomyopathy and predict survival in doberman pinschers. J Vet Intern Med. 2012; 26: 1330-1336. doi: 10.1111/j.1939-1676.2012.1000.x
32. Langhorn R, Willesen JL. Cardiac troponins in dogs and cats. J Vet Intern Med. 2016; 30: 36-50. doi: 10.1111/jvim.13801
33. Adin D, DeFrancesco TC, Keene B, et al. Echocardiographic phenotype of canine dilated cardiomyopathy differs based on diet type. J Vet Cardiol. 2019; 21: 1-9. doi: 10.1016/j.jvc.2018.11.002
34. Banton S, Baynham A, Pezzali JG, von Massow M, Shoveller AK. Grains on the brain: A survey of dog owner purchasing habits related to grain-free dry dog foods. PLoS One. 2021; 16: e0250806. doi: 10.1371/journal.pone.0250806
35. Shalamoff A, Claremont C, Miller C, Neiman N. Kibble me this: The scientific and cultural debate over boutique, exotic, and grain-free canine nutrition. 2019. https://core.ac.uk/download/pdf/289019761.pdf. Accessed January 25, 2023.
36. Dunn S. Development and Management of Canine Adverse Food Reactions and its Connections to the Grain-Free Dog Food Movement. 2020. https://digitalcommons.liberty.edu/cgi/viewcontent.cgi?article=2020&context=honors. Accessed January 25, 2023.
37. Ontiveros ES, Whelchel BD, Yu J, et al. Development of plasma and whole blood taurine reference ranges and identification of dietary features associated with taurine deficiency and dilated cardiomyopathy in golden retrievers: A prospective, observational study. PLoS One. 2020; 15: e0233206. doi: 10.1371/journal. pone.0233206
38. Wilfart A, Montagne L, Simmins PH, van Milgen J, Noblet J. Sites of nutrient digestion in growing pigs: Effect of dietary fiber. J Anim Sci. 2007; 85: 976-983. doi: 10.2527/jas.2006-431
39. Twomey LN, Pethick DW, Choct M, et al. The use of exogenous feed enzymes in reducing the anti-nutritive effects on dietary fibre in dog foods. Recent Advances in Animal Nutrition. 2001; 13: 179-186.
40. Ko KS, Fascetti AJ. Dietary beet pulp decreases taurine status in dogs fed low protein diet. J Anim Sci Technol. 2016; 58: 29.
doi: 10.1186/s40781-016-0112-6
41. Sanderson SL, Gross KL, Ogburn PN, et al. Effects of dietary fat and L-carnitine on plasma and whole blood taurine concentrations and cardiac function in healthy dogs fed protein-restricted diets. Am J Vet Res. 2001; 62: 1616-1623. doi: 10.2460/ajvr.2001.62.1616
42. Basili M, Pedro B, Hodgkiss-Geere H, Navarro-Cubas X, Graef N, Dukes-McEwan J. Low plasma taurine levels in English cocker spaniels diagnosed with dilated cardiomyopathy. Journal of Small Animal Practice. 2021; 62: 570-579. doi: 10.1111/jsap.13306
43. Huxtable RJ. Physiological actions of taurine. Physiol Rev. 1992; 72: 101-163. doi: 10.1152/physrev.1992.72.1.101
44. Sanderson SL. Taurine and carnitine in canine cardiomyopathy. Vet Clin North Am Small Anim Pract. 2006; 36: 1325-1343, vii-viii.
doi: 10.1016/j.cvsm.2006.08.010
45. Keene B, Panciera D, Atkins C, Regitz V, Schmidt M, Shug A. Myocardial L-carnitine deficiency in a family of dogs with dilated cardiomyopathy. J Am Vet Med Assoc. 1991; 198: 647-650.
46. Neumann S, Welling H, Thuere S, Kaup FJ. Plasma L-carnitine concentration in healthy dogs and dogs with hepatopathy. Vet Clin Pathol. 2007; 36: 137-140. doi: 10.1111/j.1939-165x.2007.tb00199.x
47. Rizos I. Three-year survival of patients with heart failure caused by dilated cardiomyopathy and L-carnitine administration. Am Heart J. 2000; 139: S120-S123. doi: 10.1067/mhj.2000.103917