INTRODUCTION
Optic neuritis refers to inflammation of the optic nerve. Inflammation of the optic nerve causes loss of vision usually due to the swelling and destruction of the myelin sheath covering the optic nerve. Direct axonal damage may also play a role in nerve loss in many cases. The most common aetiology in adults is multiple sclerosis (MS) while that in children is considered to be parainfectious.
Symptoms of optic neuritis include sudden loss of vision with an afferent pupillary defect in the involved eye, pain on movement of affected eye, and impairment of visual functions such as color vision, contrast sensitivity and visual fields. Typically, there is spontaneous recovery of vision and this has been shown to get accelerated by steroids.
Optic neuritis affects children less commonly than adults. Optic neuritis in children may occur as an isolated episode having, presumably, a self-limited course and carrying no prognostic implication with respect to the rest of the nervous system. Other cases may be followed by development of MS, neuromyelitis optica (NMO) or Schilder’s disease. Majority of the information about pediatric optic neuritis comes from western literature and the data is sparse in Asian countries. Furthermore, since optic neuritis treatment trial (ONTT) excluded patients with pediatric optic neuritis, little is known about its spectrum and outcome.1 It has been observed that the clinical profile and outcome of optic neuritis among adults in the Western population differs significantly from that in the East and this may hold true for pediatric optic neuritis.2
The purpose of this study is to retrospectively review the cases of optic neuritis among a population of less than 20 years of age at a tertiary care hospital in order to understand the various clinical aspects of these patients and compare it with the Caucasian population.
MATERILAS AND METHODS
A retrospective study was performed on all patients <20 years of age who presented with optic neuritis at the neuro-ophthalmology clinic of a tertiary care Apex Eye Hospital in New Delhi, India over a 3 year period. The upper age limit used to define the pediatric population varies among experts, including adolescents and up to the age of 21 is consistent with the definition found in several well-known sources.3-5 The study was approved by the Institutional Review Board. Retrospective review of the medical records of patients with a diagnosis of optic neuritis that came to a tertiary care centre during a 2 year period was done. Searches identified a total of 29 consecutive cases that were eligible for inclusion. One patient developed transverse myelitis early on follow-up and was therefore excluded from the analysis.
The diagnosis of optic neuritis was made clinically on the basis of an acute or sub-acute vision loss in one or both eyes with one or more of the following findings; pain on eye movements, optic nerve swelling, relative afferent pupillary defect in unilateral cases, dyschromatopsia, abnormal visual evoked potentials, and no other identifiable cause. The patients with neurological findings, acute disseminated encephalomyelitis or other central nervous system (CNS) causative etiology, neuroretinitis, compressive or infiltrative optic neuropathies and Leber’s hered itary optic neuropathy were excluded. Patients with other concurrent ophthalmic ailments (other than refractive error) were also excluded.
Demographic and clinical information collected for each patient included age at onset, gender, ethnicity, best corrected visual acuity at presentation, prodromal symptoms, preceding illnesses, ocular examination, relevant laboratory findings (where available/done: hemogram with ESR, serum electrolytes, quantiferon gold assay for mycobacterium tuberculosis, blood culture and sensitivity, where appropriate and autoimmune workup including antinuclear antibodies (ANA), antineutrophil cytoplasmic antibody (ANCA) and radio frequency (RF), where appropriate), perimetry, visual evoked potential (VEP), neuro-imaging, treatment, and follow-up data. Abnormal magnetic resonance imaging (MRI) was defined by the presence of one or more T2-hyperintense lesions on brain MRI.
Bilateral optic neuritis was defined as, both eyes involved simultaneously or within 4 weeks of each other, and recurrent optic neuritis was diagnosed when the repeat attack affected one or both eyes after an interval of more than 4 weeks. This is similar to the criterion used for the diagnosis of 2 demyelinating episodes/attacks in MS patients.6
Patients were subgrouped on the basis of age and gender, and the subgroups were then compared for various clinical parameters.
An excel spreadsheet was designed to collect the data and statistical analyses were performed using the SPSS (version 14.0; SPSS Inc., Chicago, IL, USA). Qualitative data were expressed as percentages and quantitative data were expressed as mean±standard deviation or median and range. Data with parametric distribution were analyzed using the Mann Whitney Utest and those with non-parametric distribution were analyzed using the Chi Square test. A p-value of <0.05 was taken as statistically significant.
RESULTS
The study included 28 patients (44 eyes) who had presented to the neuro-ophthalmology clinic over a 3 year period with a mean follow-up of 6.3±4.9 months (0.3-38 months). The mean age of
the study patients was 12.6±4.9 years (2-20 years). There were 19 males (67.9%) and 9 (32.1%) females. Two children were below 5 years of age.
A review of the past medical history revealed no significant ophthalmic disorders, injuries or illnesses. None of the patients were under any medication, there were no known drug allergies and all of them were fully immunized for their age. There was no family history of ophthalmic disease. The neurological examination was normal except for the optic nerve abnormalities. Laboratory tests showed leukocytosis in 2 patients. All other laboratory tests were negative.
The clinical features of the patients are summarized in Table 1. The mean baseline visual acuity of the study patients was 1.80±0.6 logMAR units and the last best visual acuity was 0.43±0.4 log units. 36 eyes (81.8%) had a visual acuity at or below 3/60 and 40 eyes (90.9%) had a visual acuity of 6/60 or lower of the Snellen chart at the time of initial presentation. Four patients had no perception of light at presentation (Figure 1). Overall, the visual acuity loss was severe in majority of our patients (Table 2). Papillitis was present in 20 patients (71.4%) (Figure 2). The remaining patients had normal fundi (retrobulbar neuritis (RBN)). The presentation was bilateral in 16 (57.1%) patients. Of these patients with a bilateral presentation, 87.5% (12 patients) had papillitis.
| Table 1: Clinical Features of Patients with Optic Neuritis at Presentation. |
|
Clinical features
|
Total (% Total)
|
| No. of patients |
28 (100%)
|
| Male(M) |
19 (67.9%)
|
| Female(F) |
9 (32.1%)
|
| F/M ratio |
0.47
|
| Age at onset |
12.64±4.95 years ( 2-20 years)
|
| Country of birth-India |
28 (100 %)
|
| Family history of MS |
00
|
| Eye involvement |
|
| Unilateral |
12 (42.8%)
|
| Bilateral |
16 (57.1%)
|
| Associated symptoms |
|
| Pain with ocular movements |
12 (42.9%)
|
| Other neurologic symptoms |
00
|
| Viral prodrome |
6 (21.4%)
|
| Recent immunization |
00
|
| No. of affected eyes |
44 (100%)
|
| Pupils- presence of RAPD |
12 (27.2%)
|
| Fundoscopy |
|
| Disc edema
Normal (Retrobulbar neuritis) |
34 (77.3%)
10 (22.69%)
|
| Visual fields
Abnormal
1.Central scotoma
2. Centrocecal scotoma
3. Enlarged blind spot
4. Peripheral constriction of fields
Not recordable |
18 (40.91%)
05 (11.36%)
07 (15.92%)
04 (9.09%)
02 (4.54 %)
26 (59.09%)
|
| VEP abnormal |
44 (100%)
|
| Follow-up |
6.38±4.99 months
(Range 0.25-38 months)
|
| Table 2: Visual Acuity in 28 Patients of Pediatric Optic Neuritis (44 Eyes). |
|
Visual acuity (LogMAR)
|
Snellen equivalent visual acuity |
Initial VA (Number of eyes (n) ) |
Best attained VA (Number of eyes (n))
|
|
0.3 or better
|
6/12 or better |
1 |
27
|
|
<0.3-1
|
<6/12-6/60 |
7 |
13
|
|
<1-1.3
|
<6/60- 3/60 |
1 |
0
|
|
<1.3-1.77
|
<3/60-1/60 |
5 |
3
|
|
<1.77
|
<1/60 |
30 |
1
|
|
Total
|
44 |
44
|
Figure 1: Visual Acuity at Presentation.
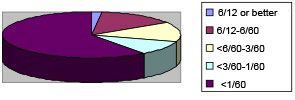
Figure 2: Fundus Image of a Case of Papillitis, Taken on a Portable Smartscope Pro (Optomed Oy, Finland) Fundus Camera.
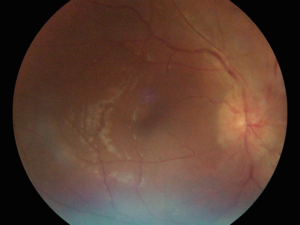
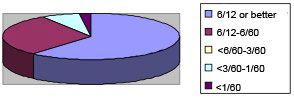
All the patients were given pulse dexamethasone (3-5 mg/kg/d) for three consecutive days followed by oral prednisolone (1-1.5 mg/kg/day) for 11 days. This was in accordance with the treatment guidelines of the institution where all pediatric optic neuritis patients are given steroids after the baseline investigations rule out an infective etiology. This is to ensure a quicker visual recovery as majority of these cases are bilateral and have profound visual loss. Also, pulse dexamethasone is used in view of better safety and equal efficacy to IV methylprednisolone (as used in optic neuritis treatment trial).7 The visual acuity improved in all the patients. At 1 week, 21 out of 44 eyes (47.7%) had a visual acuity ≥6/18 of the Snellen chart (Figure 3). Post-treatment assessments were individualized for each patient. Generally, the assessments were done at 1 week, 1 month, 1 month, 3 months and 6 monthly thereon. All the patients who recovered to a VA of 6/6 continued to have some amount of disc pallor. The final visual acuity of patients with RBN was 0.504±0.59 (median of 0.2) and in papillitis was 0.408±0.40 (median of 0.3) and the difference was not statistically significant (p=0.83) A total of 9 eyes (20.5%) of 6 patients (20.7%) had a recurrence. Of these, five patients had retrobulbar neuritis and one had papillitis. The median period of recurrence was 2 months (0.5-9 months).
Figure 3: Visual Acuity at Final Follow-up.
MRI was done in 19 patients (67.8%). MRI showed absence of any demyelinating lesions in the brain (other than the optic nerve) in 14 patients, 3 patients showed lesions suggestive of MS. These patients were 7, 12 and 15 years old and had demyelinating lesions in the brain (other than the optic nerve) at only one of the four typical locations in MS (periventricular, infratentorial, juxtacortical and spinal cord).5 VEP was done in all the patients and demonstrated increased latency of the p100 wave in all the patients (mean amplitude of 5.5 microvolt and latency 132 msec). Visual fields (Goldmann visual perimetry or GVF) could be charted in 18 eyes and centrocecal/central scotoma was the most common field defect (Table 1).
Nine patients were below 10 years of age. Subgroup analysis of patients aged 0-11 years and 11-20 years is depicted in Table 3. Those below 11 years of age presented more commonly with papillitis (p=0.01) and had bilateral disease, though the difference was not statistically significant (p=0.054). The males and females were very similar in relation to age, laterality, pain on ocular movements, mean baseline and best achieved visual acuity, mean contrast sensitivity, disc edema and recurrences.
| Table 3: Subgroup Analysis of Pediatric Optic Neuritis Patients According to Age (n=28 Patients). |
|
Age≤10 years (n=9 patients/17 eyes)
|
Age=11-20 years (n=19 patients/27 eyes) |
p value (test used)
|
| Number of males |
4/9
|
5/19 |
0.599 (Chi square test)
|
| Bilateral |
8/9
|
8/19 |
0.054 (Chi square test)
|
| Pain on ocular movements |
2/9
|
10/19 |
0.267 (Chi square test)
|
| Baseline visual acuity |
1.84±1.1
|
1.77±1.3 |
0.632 (Mann whitney test)
|
| Baseline contrast sensitivity |
1.09±0.36 |
0.97±1.14 |
0.88 (Mann whitney test)
|
| Number of patients with papillitis |
17/17
|
17/27 |
0.013 (Mann whitney test)
|
| Best visual acuity achieved |
0.37±0.44
|
0.46±1.12 |
0.49 (Mann whitney test)
|
| No. of patients with improvement in visual parameters |
10/17
|
17/27 |
1.00 (Chi square test)
|
| Recurrence |
0/9 |
6/19 |
0.159 (Chi square test) |
DISCUSSION
In this series, we retrospectively reviewed the medical records of optic neuritis patients, and found 28 patients fitting the eligibility criterion. While this number appears small, pediatric optic neuritis forms nearly 5% of the patients with optic neuritis and this is similar to that reported from the West.8 Two children were below 5 years of age. Such an early presentation is increasingly been reported. Visudhiphan et al9 reported cases between 1-2 years of age.The female to male ratio of our study patients was 0.47. This is in contrast to the female preponderance in adult optic neuritis and also the majority of the pediatric optic neuritis studies.10-19 However, Hwang et al13 also did not find a female predilection in Korean children.
History of a viral prodrome is a common finding in children and differentiates it from adult cases. We could document the history of viral prodrome in 6 (21.4%) patients. Wilejto et al12 documented viral prodrome in 28% of the optic neuritis patients. Kennedy et al10 suggested that there is no significantly better visual prognosis in children having retrobulbar neuritis as opposed to those having papillitis. The best corrected visual acuity was similar in patients with papillitis and RBN in our study.
Bilateral involvement, which is common in children with optic neuritis, is present in only about one-third of the adults. In our study, 16 patients (57.1%) had a bilateral presentation. Children below 10 years of age more commonly had a bilateral presentation, though this was not statistically significant (p=0.054). The published data has quoted 42-100% of the pediatric patients to have a bilateral presentation.10-20
A second noteworthy ocular finding in pediatric optic neuritis is the large number of patients who had papillitis. Kennedy et al10 noted that more than 70% of the children had some degree of papillitis, normal discs being noted in only three cases (10%). Other studies have also reported papillitis in as many as 87% of pediatric cases.21,22 In our study, 77.3% of the eyes had papillitis as the presenting feature. All the eyes (100%) presenting below 10 years of age had papillitis.
Children with optic neuritis carry a relatively low risk of subsequent neurologic disease (13% risk of MS by 10 years of age, 19% by 20 years of age, 22% by 30 years of age, and 26% by 40 years of age).13,18-23 Recurrences were noted in 6 eyes of 9 patients in this study. Of these, MRI of 3 patients showed lesions suggestive of MS but did not confirm to the diagnosis of clinically definite MS and was diagnosed as ‘Probable MS’. It is difficult to predict the risk of MS because of a shorter follow-up and needs a long-term study.
A comparison of the clinical profile and risk of multiple sclerosis of Indian patients and Caucasian population has been shown in Table 4.
| Table 4: Table Depicting Comparison of Caucasian Population and Indian Population with Regard to Clinical Profile of Pediatric Optic Neuritis. |
|
Parameter
|
Wan et al25 |
Jayakody et al26 |
Wilejto et al27 |
Bonhomme et al28 |
Alper et al29 |
Current Study
|
|
Country
|
USA |
USA |
Canada |
USA |
USA |
India
|
|
Number of cases
|
46 |
26 |
36 |
29 |
30 |
28
|
|
Age
|
12.6 (3.9-18.8) |
11.2 (4.5-19) |
12.2 (2.2-17.8) |
9.6(4.3-16) |
10.2 (3.4-16.9) |
12.6 (2-20) |
|
M:F ratio
|
13:33 |
6:19 |
5:30 |
8:21 |
14:16 |
19:9
|
|
Unilateral:Bilateral
|
27:19 |
14:12 |
21:15 |
13:16 |
20:30 |
12:16
|
|
Papillitis
|
31 |
19 |
NA |
NA |
12 |
4
|
|
Multiple Sclerosis
|
18 |
2 |
14 |
3 |
6 |
3
|
To conclude, pediatric optic neuritis patients are present with poor vision but are associated with a good visual outcome and a faster recovery. There are no gender differences in either the presentation or the visual recovery. Papillitis was more often seen in the children below 10 years of age. None of the patients developed clinically definite MS.
DISCLAIMER
There is no conflict of interest, financial or otherwise with regard to this study.
Vision at presentation was poor in most children with over 90% having a visual acuity of 6/60 or lesser. The vision loss as well as the recovery was similar in male and females (0.62 and 0.57 respectively). Visual recovery was good with 40 eyes (90.9%) gaining a visual acuity of more than 6/60 and 27 eyes (61.4%) gaining more than 6/12 at an average follow-up period of 6.38 months. Children below 10 years of age had a visual recovery similar to those between 11-20 years of age (p=0.49). Kriss et al14 reported a visual acuity of 6/6 or better in 90% of the patients at 8.8 years of follow-up, Wan et al19 too reported good visual outcomes with nearly 90% regaining 20/40 or better vision and a study from Thailand has shown 70% cases to have complete visual recovery.20 Malay children have been shown to have a worse visual outcome in a recent study.18








