SUMMARY
Oral submucous fibrosis (OSMF or OSF) is a severely debilitating oral premalignant condition characterized by restricted mouth opening secondary to formation of fibrous bands due to deposition of collagen in the submucosal connective tissue and fibrosis of the lamina propria.1,2 In severe cases the oral opening is less than 15 mm and presents difficulty in oral hygiene care and dental care.3 Trismus and decreased laxity of buccal soft tissues make these patients poor candidates for any dental treatment and often present with multiple decayed teeth and periodontal problems. Fracture management in these patients is often challenging. The present case reported with a bilateral compound fracture of mandible due to a road traffic accident. Open reduction and internal fixation was done. The trismus due to oral submucous fibrosis in the patient needed certain treatment modifications which have been reported. Online search for “jaw fracture management in oral submucous fibrosis patients” yielded no results. This paper thus seems to be the first account on the management of such patients in English literature.
INTRODUCTION
Oral submucous fibrosis (OSMF or OSF) is a premalignant condition widely prevalent among areca nut and tobacco chewing population characterized by formation of dense avascular collagenous deposits within the submucosal layers in the connective tissues. Continual habit leads to a relentless progression and significant morbidity and mortality. In severe cases progressive fibrosis results in severely restricted mouth opening and a high risk of squamous cell carcinoma development.
CASE REPORT
The present case reported with a bilateral compound fracture of body of mandible due to a road traffic accident. Occlusion was deranged due to overriding of fracture segments. The patient had a class III malocclusion with a reverse over jet. The oral opening was restricted to about 20 mm (Figure 1). The patient was recorded with a history of pan masala chewing (contains areca nut and lime) for about 8 years with a gradual reduction of mouth opening. Other sign and symptoms of OSMF were also present such as intolerance to spices and hot food items, reduced tongue protusion, difficulty in chewing and compromised oral hygiene care.
Figure 1: Restricted Oral Opening.
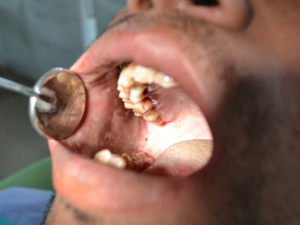
Maxillo-mandibular fixation (MMF): Stiffness and reduced laxity of buccal soft tissue made digital buccal retraction impossible. Hence wiring for MMF required that wires be passed from palatal/lingual interdental spaces to buccal/labial interdental (Figure 1).
Incision: A modified intraoral vestibular incision was used to access the body region. The approach was extended posteriorly for better access to the body and angle region.
Between the canines the incision was made 20-25 mm (normally 10-15 mm) away from the attached gingiva in a curvilinear fashion. In the body region the incision was kept superior to the mental nerve. Posterior to the canine the incision was kept 8-10 mm away from the attached gingiva, staying superior to the mental nerve. Fibrotic bands present at this point were incised to aid in retraction of soft tissues. The branches of the mental nerve located just underneath the mucosal flap were skeletonised by spreading scissors parallel to nerve. This was done to aid in retraction and to access the fracture line distal to the mental foramen.
Fracture reduction and fixation: Fracture reduction and fixation was done with 2.0 mm titanium system, Synthes Corporation Pvt. Ltd., West Chester, PA, USA. Two screws of 8 mm length were placed on each side of the fracture line.
Combination with the transbuccal technique: To place posterior screws minimizing mental nerve retraction, the transbuccal trocar was used to drill holes and keep the screws perpendicular to the plate.
Wound closure: The incision was closed after thoroughly irrigating the wound and checking for hemostasis. Anteriorly, the mentalis muscle was reapproximated to prevent drooping of the chin tissues. The mucosa was closed with interrupted 3-0 vicryl resorbable sutures. An elastic pressure dressing on the chin region was given to help support the soft tissues and prevent hematoma formation (Figures 2, 3 and 4)
Figure 2: Maxillo-Mandibular Fixation with Lingual Insertion of Wires.
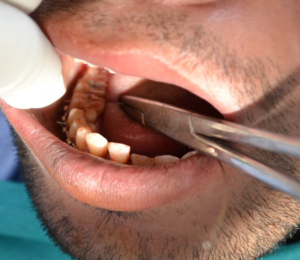
Figure 3: Open Reduction and Internal Fixation.
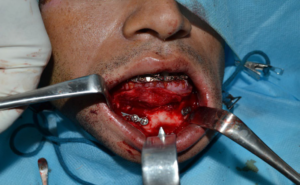
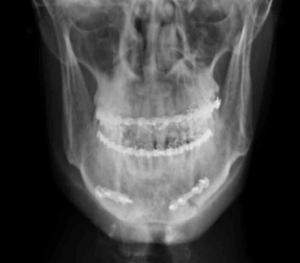
Figure 4: Post-Operative Radiograph Showing Miniplates Osteosynthesis.
Oral submucous fibrosis (OSMF) is a chronic, irreversible, highly potent pre-cancerous condition characterized by juxta-epithelial inflammatory reaction and progressive fibrosis of the submucosal tissues. It is thought to be an oral pre-cancerous condition with about 7.6% malignant transformation rates. The histopathological hallmark of the disease is fibrosis that affects most parts of the oral cavity, pharynx and upper aero digestive tract. Intolerance to spicy food, rigidity of lip, tongue and palate leading to varying degrees of limitation of opening of the mouth and tongue movement.3 In severe cases the oral opening is less than 15 mm and presents difficulty in oral hygiene care and dental care. Trismus and decreased laxity of buccal soft tissues make these patients poor candidates for any dental treatment and often present with multiple decayed teeth and periodontal problems. Fracture management in these patients is often challenging. Conservative management by closed reduction and maxillo-mandibular fixation is also difficult due to fibrous bands and inelastic buccal tissues with limited cheek retraction. Placement of wires from palatal/lingual to buccal/labial interspaces need to be done with smaller head wire twisters.
The intraoral vestibular incisions are the usual access for simple fractures of the symphysis, parasymphysis and body region. The approach can be extended posteriorly for better access to the body and angle region. Between the canines the incision was made 20-25 mm (normally 10-15 mm) away from the attached gingiva in a curvilinear fashion. Friability and ease at tearing of fibrosed, avascular mucosal and submucosal tissue meant that an increased bulk was required to aid in wound closure later on. In the body region the incision was kept superior to the mental nerve. Particularly in the extended intraoral approach such as this, care must be taken to protect the mental nerve in the anterior body region. Posterior to the canine the incision was kept 8-10 mm mm away from the attached gingiva, staying superior to the mental nerve. Fibrotic bands present at this point were incised to aid in retraction of soft tissues. The branches of the mental nerve located just underneath the mucosal flap were skeletonised by spreading scissors parallel to nerve. This was done to aid in retraction and to access the fracture line distal to the mental foramen.
Mandibular fracture fixation in the symphysis and body region often can be done intraoral approach but fractures distal to the foramen area often require a transoral approach.4,5 Placement of screws which are distal to mental foramen may require a transbuccal trocar in order to keep the screws perpendicular to the plate.
Wound closure has to be done in layers with greater importance to reattachment of muscular tissue. Decreased vascularity of the mucosal and submucosal connective tissues can present with problem in healing especially at wound edges which mandates that the wound edges to be kept everted during suturing.
CONCLUSION
Fracture management in an oral submucous fibrosis patient even though challenging but can be done with certain modifications as elaborated in this case.
CONFLICTS OF INTEREST
The authors declare that they have no conflicts of interest.
CONSENT
An informed consent was taken from the patient prior to surgery and also prior to submission.









