INTRODUCTION
A Miller-Fisher syndrome is a rare clinical variant of Guillain-Barré syndrome, an acute immune-mediated neuropathy that is the most common cause of acute paralysis worldwide.1 Both Miller-Fisher syndrome and Guillain-Barré syndrome are thought to generally be either prompted by viral or microbial components or by molecular mimicry via a cross-reaction between infectious pathogens and peripheral nerve gangliosides, yielding anti-ganglioside antibodies; however, only 76% of patients have a known antecedent event.2,3 Miller Fisher syndrome is often suspected in patients with two of the three integral components of the Miller-Fisher syndrome triad: ophthalmoplegia, ataxia, and areflexia. In contrast to the ascending motor paralysis and limb involvement in Guillain-Barré syndrome, Miller-Fisher syndrome manifests in a descending pattern, beginning with dysfunction of CN III, IV and VI.2 However, there may be an overlap between the two polyneuropathies when the motor weakness of the limbs and the respiratory system are involved in addition to the triad.2 In Miller-Fisher syndrome, there are also reports of autonomic dysfunctions across the Guillain-Barré syndrome spectrum, including cardiac manifestations.4 Due to its rarity, little research has been conducted regarding the appropriate treatment of Miller-Fisher syndrome—especially mild Miller-Fisher syndrome; standard Guillain-Barré syndrome treatments are typically pursued in patients with possible Miller-Fisher syndrome in the absence of known efficacy due to clinical overlap between the two conditions, with intravenous immunoglobulin being preferred clinically over plasma exchange in practice.3,5
CASE PRESENTATION
A 63-year-old female with uncontrolled type II diabetes (T2Ds), chronic obstructive pulmonary disease, depression, essential hypertension, iron deficiency anemia, and allergic rhinitis presented to the emergency department with a 2-day history of the right arm and bilateral leg weakness, a 1-week history of the right hand and left fifth finger neuropathy, a 1-month history of bilateral foot neuropathy, and worsening balance and blurry vision for an indeterminate amount of time, with no associated aggravating or alleviating factors noticed by the patient. The patient was at her baseline otherwise, with no recent fever, chills, nausea, vomiting, diarrhea, shortness of breath, cough, or other infection symptoms; moreover, the patient denied any recent immunizations too. The patient’s social history was unremarkable, with no history of smoking, drinking, or illicit substance use.
Vitals were within normal limits in the emergency department aside from elevated blood pressure; the patient was afebrile with normal heart and respiratory rates. The initial physician exam in the emergency department was significant for decreased left eye abduction with associated dysconjugate gaze; strength and sensation were intact and equal in bilateral upper and lower extremities, with no reflexes documented at the time.
After admission, symptoms progressed to include impaired right eye abduction and left eye nystagmus, as well as areflexia and dysmetria, while left eye abduction difficulties appeared to have resolved. The musculoskeletal exam was frequently inconsistent, with poor patient effort and multiple discrepancies noted between the physical exam and incidental observation; however, subjective and objective weakness did worsen. Blood pressure also fluctuated significantly during admission but stayed elevated despite multiple anti-hypertensive agents.
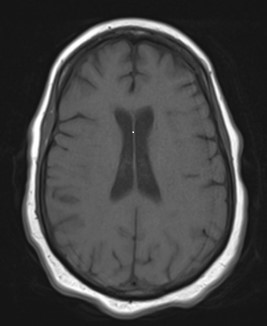
Brain magnetic resonance imaging (MRI) (Figure 1), brain computed tomography (CT) and cervical spine MRI were all unremarkable, so neurology was consulted. Per neurology’s recommendations, a lumbar puncture was obtained. See Tables 1 and 2 for results and confirmation of albumino-cytologic dissociation; of note, the GQ1b antibody results were not available until after patient discharge. Given the presence of areflexia, ataxia, and ophthalmoplegia in a negative workup, neurology recommended starting a 5-day course of intravenous immunoglobulin for presumptive Miller-Fisher syndrome. Symptoms continued to worsen on intravenous immunoglobulin treatment until Day 5 of treatment, when the patient experienced a significant objective improvement in weakness from 1/5 to 4/5 of bilateral upper and lower extremities and a significant subjective improvement in diplopia. However, areflexia and right eye abduction impairment did not improve. Electromyogram results were not available during the hospitalization.
Figure 1. MRI of Brain
| Table 1. Serum Results |
| Immunoglobulin G, serum |
1230 mg/dL |
| Albumin, serum |
4.1 g/dL |
| GQ1b Antibody |
<1:100 |
| Albumino-cytologic dissociation demonstrated |
| Table 2. Cerebrospinal Fluid Results |
| Color |
Colorless |
| Clarity |
Clear |
| Nucleated cells |
28 |
| Red blood cell count |
242 |
| Pathology interpretation |
Normal study |
| Differential |
92% lymphocytes, 8% monocytes |
| Protein |
278 mg/dL |
| Glucose |
127 mg/dL |
| Culture |
No growth |
| Gram stain |
No organisms seen |
| Synthesis rate, immunoglobulin G, cerebrospinal fluid |
26.4 mg/ 24 h |
| Immunoglobulin G index, cerebrospinal fluid |
0.62 |
| Albumin, cerebrospinal fluid |
113.0 mg/dL |
| Immunoglobulin G, cerebrospinal fluid |
20.9 mg/d |
| Results consistent with acute demyelinating process |
DISCUSSION
Although this patient’s presentation did include the clinical triad of areflexia, ataxia, and ophthalmoplegia associated with Miller-Fisher syndrome, inconsistencies in lab results, physical exam, and treatment response suggest a possible variant of the syndrome. The ophthalmologic involvement is especially striking, given the unilateral ophthalmoplegia and contralateral nystagmus, which automatically downgraded the Brighton Collaboration level of diagnostic certainty to a Level 4 due to the lack of bilateral ophthalmoplegia.6 However, the improvement in diplopia and resolution of left eye nystagmus after a 5-day course of intravenous immunoglobulin suggests this ophthalmoplegia could indeed be attributed to a Miller-Fisher syndrome-related acute vestibular syndrome with autonomic involvement as well.3,6 The cerebrospinal fluid protein is also elevated far above that usually seen in Miller-Fisher syndrome, as Miller-Fisher syndrome patients tend to have lower protein levels—even below typical Guillain-Barré syndrome levels.7 An electromyogram was not available during the initial hospitalization; however, it should be noted that such testing is neither required for diagnosis nor accessible to all patients, as was the case for this patient.6 See Table 3 for the final results of the electromyogram performed several months later, which suggest a mixed axonal and demyelinating sensory-motor neuropathy.
| Table 3. EMG Summary Table |
| Electromyogram Results |
|
Muscle
|
Nerve |
Roots |
Recruitment Pattern
|
| R. first dorsal interosseous |
Ulnar |
C8-T1
|
Reduced |
| R. abductor pollicis brevis |
Median |
C8-T1
|
Reduced |
| R. flexor carpi ulnaris |
Ulnar |
C7-T1
|
Reduced |
| R. pronator teres |
Median |
C6-C7
|
Reduced |
| R. biceps brachii |
Musculocutaneous |
C5-C6
|
Normal |
| R. triceps brachii |
Radial |
C6-C8
|
Reduced |
| R. brachioradialis |
Radial |
C5-C6
|
Normal |
| R. extensor digitorum communis |
Radial |
C7-C8
|
Reduced |
| R. deltoid |
Axillary |
C5-C6
|
Normal |
| Electromyogram suggests a mixed axonal and demyelinating sensory motor neuropathy. |
CONCLUSION
This case highlights the need for further research into Miller-Fisher syndrome and other Guillain-Barré syndrome variants, especially regarding treatment, as the response to standard intravenous immunoglobulin treatment for Guillain-Barré syndrome in this patient was incomplete. However, the low-risk associated with immunoglobulin use and this patient’s partial response do suggest that intravenous immunoglobulin may be an appropriate treatment option for patients with potential Miller-Fisher syndrome variants who may be at increased risk of further complications or who are unable to tolerate symptoms.
CONSENT
Permission to pursue publication of case report was obtained directly from involved patient on 12/1/22 by primary author via phone call at 1027 after discussion of relative risks and benefits of such a pursuit, in accordance with WVU Medicine Wheeling Hospital Family Medicine Residency’s policy on case report publications and inherent exclusion from IRB formal review process due to limited risk to patient as long as patient’s private medical information is kept confidential.
CONFLICTS OF INTEREST
The authors declare that they have no conflicts of interest.






