CASE REPORT
In this case, we describe the first reported occurrence of severe, symptomatic hypercalcemia following the use of calcium based beads placed surgically into a hip arthroplasty.
The patient’s consent for clinical history and x-rays has been obtained for the purposes of publication. A 72-year-old Caucasian female had an initial right Total Hip Arthroplasty (THA) on April 21st, 2014 (using an 11 mm high offset Taperloc Complete stemTM, 50 mm Tri-Spike acetabulumTM, 44 mm E-poly active articulation and 28 mm ceramic head) due to degenerative osteoarthritis, with operative findings of eburnated bone and severe arthofibrosis of the hip. On May 29th, 2014, she represented to the Emergency Room with severe pain in the right hip, redness along the surgical site; low grade fever (37.5 ºC) and mild leukocytosis (white blood cell (WBC) count 11 K/µL) with neutrophilia (82.8%). Initial blood cultures demonstrated no growth. She underwent a revision with a Biomet® 50 mm polyethylene Freedom acetabulumTM, 36 mm head Freedom headTM with ultra-high dose antibiotic mixture. Intraoperatively, she was found to have purulent fluid throughout the hip and subsequently grew Methicillin-resistant Staphylococcus aureus. She had recurrence of severe pain in early August 2014 and was again readmitted on August 18th, 2014, found to have leukocytosis (WBC, 17.8 K/µL) where she underwent a second revision that involved the use of a 56 mm Regenerex acetabulumTM and 190 mm Arcos STS stemTM, placed due to the previous stem. There was in duration, erythema but no obvious purulence during this procedure and subsequent cultures did not show evidence of growth. Three screws were placed for additional fixation. Antibiotic impregnated calcium sulfate beads (AICBs), using OsteosetTM beads, in this case with 2 g of Vancomycin and 3.6 g of Tobramycin, prepared by the hospital pharmacy department per company issued instructions, were implanted around and medial to the prosthesis and hip joint (Figure 1). Her post-operative course was initially complicated by Coombs positive hemolytic anemia, with a drop in hemoglobin to 4.7 g/dL for which she required several blood transfusions. Uncorrected Serum calcium levels began to increase on day 3 to 10.7 mg/dL. Calcium further increased through post-operative day 4 (13.3 mg/dL), at which time ionized calcium level was 7.55 mg/ dL, peaked on day 5 (14.5 mg/dL) before decreasing, dropping to a normal level on post-operative day 8 (Figure 2). Immediate post-operative x-ray of the hip demonstrated the radio-opaque beads around and predominantly medial to the right hip where the beads were placed. To our surprise, the beads were no longer radio-opaque on the x-ray on post-operative day 5 (Figure 1), showing near complete-absorption. The patient exhibited symptoms of acute delirium, with an unsteady gait, and confusion. Her blood pressure had been controlled with systolic pressures consistently less than 140 mm Hg, increasing to a peak of 178/72 on post-operative day 6. She was unable to participate in physical therapy. Her past medical history included osteoarthritis, anxiety, and hypertension. Post-operative medications included vitamin D supplements at 1000 IU a day, acetaminophen, diphenhydramine, fluoxetine, ketorolac, gabapentin, folacin, cyanocobalamin, pyridoxine, pantoprazole and magnesium sulfate. Her physical examination was essentially unremarkable, with a clean healing surgical wound as the only pertinent finding. A full evaluation included vitamin D profile, Parathyroid (PTH) and PTH-related peptide levels and serum protein electrophoresis (Table 1), were unrevealing. We believe that the rapid absorption of the AICBs were responsible for the occurrence of hypercalcemia corresponding with calcium levels as seen on the graph (Figure 2). She had a minor renal injury apparent in June with a creatinine that increased to 2.12 mg/dL, however, at the time of readmission in August her creatinine had improved to 1.14 mg/ dL, with minor fluctuation during this last hospital admission.
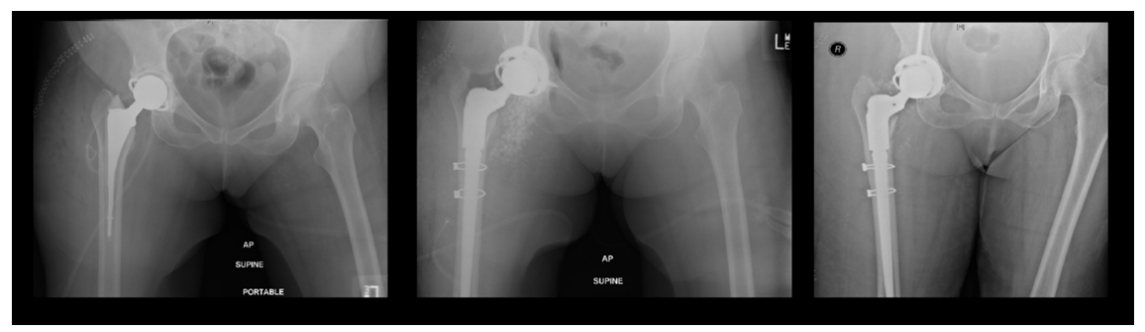
Figure 1: Series of Anteroposterior Supine X-rays, from left to right, initial film May 2014, immediately post-operatively (Aug 18th) and post-operative day 5.
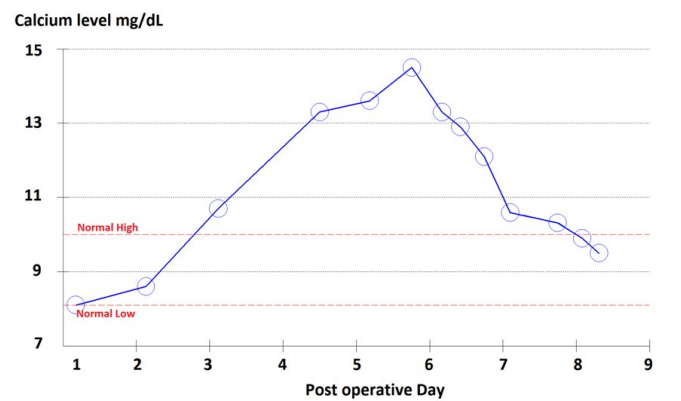
Figure 2: Calcium graph.
|
Lab
|
Value
|
Normal values
|
|
Total Uncorrected Calcium
|
13.6 mg/dL
|
8.1-10 mg/dL
|
|
25-OH-Vitamin D
|
26.4 ng/mL
|
30-100 ng/mL
|
|
1,25-OH-Vitamin D
|
13 pg/mL
|
15-75 pg/mL
|
|
SPEP
|
Negative
|
Negative
|
|
Intact-PTH
|
2.8 pg/mL
|
14-72 pg/mL
|
|
PTH-rP
|
4.3 pmol/L
|
0-3.4 pmolL
|
|
Mg
|
1.4 mg/dL
|
1.7-2.5 mg/dL
|
|
Creatinine Kinase
|
92 Units/L
|
20-155 Units/L
|
|
Phosphorous
|
2.1 mg/dL
|
2.3-4.4 mg/dL
|
|
Creatinine
|
1.16 mg/dL
|
0.5-1.2 mg/dL
|
Table 1: Laboratory values on post-operative day 5.
The patient was treated aggressively with intravenous saline, initially at a rate of 100 cc/hour and then increasing to 200 cc/hour during her highest blood calcium levels. Her hypertension was treated with amlodipine 10 mg orally daily. A single dose of calcitonin was administered of 200 IU/mL subcutaneously on post-operative day 7. Other treatment options were considered but felt inappropriate including further calcitonin dosing, bisphosphonates and loop diuretics. The patient right away responded to aggressive intravenous fluid therapy; and as the serum calcium improved, the confusion and delirium resolved. Ultimately, on post-operative day 9 she was transferred to a local rehabilitation unit. During follow visits she has done well without recurrence of pain in the hip or signs of infection.
DISCUSSION
To our knowledge, hypercalcemia has not been previously reported following the use of AICBs in any peri-prosthetic surgery. AICBs are being used more frequently in orthopedic surgery as they may act as both a bone graft substitute and provide a vehicle for local delivery of antibiotics. Methicillin-resistant Staphylococcus aureus (MRSA) dominates the infectious pathogens in post-operative orthopedic surgery, for which local delivery of antibiotics, such as Vancomycin, have the potential to significantly improve patient outcomes. Manufacturers of AICBs warn of possible transient hypercalcemia when using the product, however have not quantified this risk. Studies using AICBs in the past have shown absorption rates of ⁓93% at 1 month and 100% at 3 months.1 In contrast to these reports, x-rays taken on post-operative day 5 showed near complete absorption at the surgical site. Our x-rays, coupled with the dramatic rise in serum calcium, indicate an unambiguous correlation between hypercalcemia and the absorption of the AICBs, in the setting of an otherwise unremarkable serological evaluation. The patient developed an acute encephalopathy secondary to the hypercalcemia that prevented participation in standard post-operative physical therapy and presented a significant fall and aspiration risk.
It is unclear why the beads underwent such uncharacteristically rapid absorption in this case. Our team speculates that this may be due to the placement of the majority of the beads in adjacent vascular soft tissue, or a potential interaction between the antibiotics and the beads, that increased solubility. The dosing may have been liberal, although this in itself should not have affected the rate of absorption but rather the degree of hypercalcemia.
Recommendations for using AICBs in future cases include monitoring serum ionized calcium levels for the days following the procedure, in addition to pre- and post-operative tests for renal function, phosphate levels and post-operative evaluation hypercalcemic symptoms. In cases where the hypercalcemia cannot be ameliorated by fluids alone, other potential therapies such as loop diuretics or even hemodialysis may need to be considered.
Hip arthroplasty is a common surgical procedure, with an estimated 168,000 cases in individuals over the age of 65 in 2010.2 By 2030, the number of procedures in the United States is projected to increase by 174% to nearly 600,000 procedures per year, while hip revision procedures are expected to double by the year 2026;3 furthermore, MRSA infections in periprosthetic surgeries have had a historic occurrence of 1-2% in primary surgeries and rises to 3-4% in revision surgeries1,4 and with the rise in the procedures the use of AICBs are also expected to increase. The combination of calcium beads with antibiotics is an off-label use and guidelines for AICBs are only specified for the use of the calcium beads alone. The mechanism of the rapid absorption of the calcium in our case is currently unknown, and we further recommend more studies on absorption rates of AICBs following the addition of antibiotics by manufacturers.
DECLARATIONS: None.







